That sharp, sudden pain you feel when you drink something cold or eat something sweet? That’s tooth sensitivity, and it’s a problem that affects nearly half of all adults. It all starts with a layer of your tooth you might not even know about: the dentin.
Think of dentin as the sensitive core just beneath your hard, protective enamel. It's filled with thousands of tiny, fluid-filled tubes that act like microscopic straws leading straight to your tooth's nerve. When the enamel wears down or your gums pull back, these tubes are exposed. Suddenly, things like ice cream or hot coffee can rush down these channels and send a direct shockwave to the nerve. It’s an uncomfortable experience, but understanding the cause is the first step toward finding a solution.
Uncovering The Root Causes Of Tooth Sensitivity
So, what causes this protective barrier to fail? It almost always boils down to one of two problems: your enamel is wearing away, or your gums are receding. Both pathways lead to the same destination—exposed dentin and that all-too-familiar jolt of pain.
Enamel Erosion: When Your Tooth’s Armor Thins Out
Your enamel is the hardest substance in your body, but it’s not invincible. Over time, things like acidic foods and drinks (think citrus, soda, and wine), brushing too aggressively with a hard-bristled brush, or even grinding your teeth at night can slowly wear it down. As the enamel thins, those sensitive dentin tubules underneath become vulnerable to the outside world, leading to discomfort.
Gum Recession: When The Protective Seal Is Broken
Your gums are supposed to form a tight seal around your teeth, protecting the sensitive root surfaces. But if your gums start to pull back—a process called gum recession—they uncover the tooth roots, which don't have a thick layer of enamel to protect them. Gum disease, aggressive brushing, or even just natural aging can cause gums to recede, leaving the roots exposed and highly sensitive.
This simple breakdown illustrates how different habits and conditions can lead to that painful sensitivity.
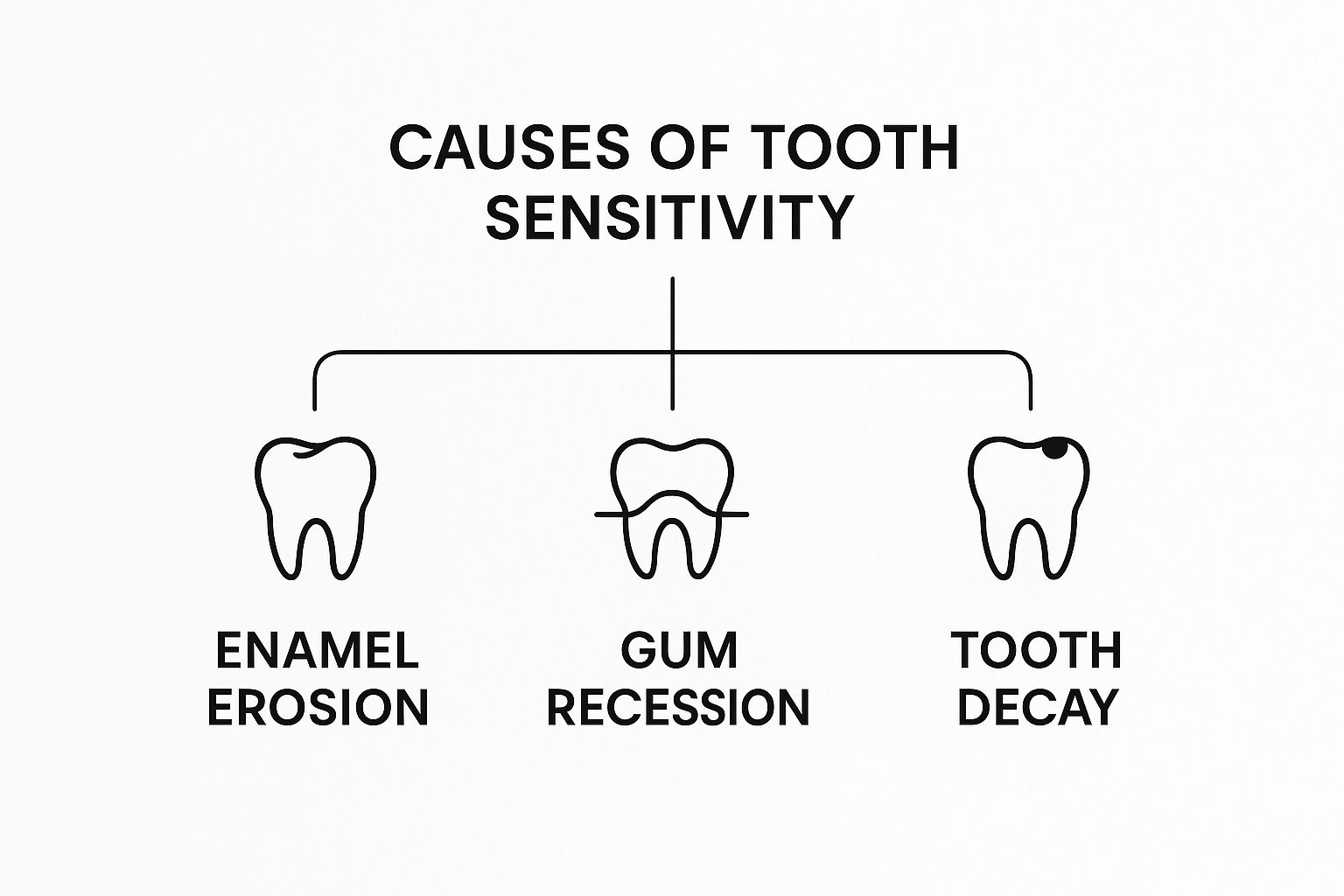
To make it even clearer, let's look at the two main culprits behind sensitive teeth and how they expose the nerve.
The Two Main Pathways to Tooth Sensitivity
| Cause | How It Exposes Nerves | Common Triggers |
|---|---|---|
| Enamel Erosion | Wears down the tooth's hard, protective outer layer, revealing the porous dentin beneath. | Acidic foods, aggressive brushing, teeth grinding (bruxism). |
| Gum Recession | The gum tissue pulls away from the teeth, uncovering the sensitive root surface that lacks enamel protection. | Gum disease, harsh brushing techniques, smoking, genetics. |
These two issues are incredibly common. Research shows that gingival recession is a factor in about 66% of tooth sensitivity cases, while enamel wear is right behind it, contributing to 59% of cases. The numbers don't lie—protecting your enamel and gums is your best defense.
Pain is your body's alarm system, and ignoring it only gives the underlying problem more time to get worse. Understanding why you shouldn't ignore a sensitive tooth is the first step toward finding relief and keeping your smile healthy for the long haul.
How Your Everyday Habits Might Be Weakening Your Enamel
It’s strange to think that things we do every single day could be setting us up for that sharp, sudden pain of tooth sensitivity. But often, that’s exactly what’s happening. The most common cause is the slow, steady wearing away of your tooth enamel, and our habits are usually the main culprits.
This breakdown of your enamel shield typically happens in two key ways. First, there's the chemical attack from what we eat and drink. Then there's the mechanical wear and tear from how we care for our teeth. Getting a handle on both is the first step to keeping that painful zing at bay.
The Problem with Acidic Foods and Drinks
A lot of the foods and drinks we love are, unfortunately, quite acidic. Over time, that acid can literally soften and dissolve the hard, protective enamel on your teeth. Once the enamel thins out, the next layer down—a more porous and sensitive layer called dentin—is exposed. That’s when you start feeling those jolts of pain.
You'd be surprised what's on the list of common offenders:
- Sodas and Sports Drinks: Many are packed with acids like phosphoric and citric acid.
- Citrus Fruits: Lemons, limes, and oranges are great for your health but can be tough on your teeth.
- Coffee and Wine: Both of these popular drinks are acidic enough to weaken that crucial outer layer of your teeth.
It’s not about giving these things up entirely, but a little mindfulness goes a long way. Simply rinsing with water after you have something acidic can help neutralize the attack. If you want to dive deeper, check out this guide to the most acidic beverages and foods to limit or avoid.
Are You Brushing Too Hard?
It’s not just about what you put in your mouth; it’s also about how you clean up afterward. If you’re a vigorous brusher, you might be doing more harm than good. Brushing too aggressively can physically scrub away your enamel, a problem that’s especially common right at the gumline where the enamel is already thinner.
The type of brush you use matters, too. A toothbrush with hard or even medium bristles can act like sandpaper on your teeth, creating the same abrasive damage. Remember, the goal is to gently clean away plaque, not to scour your teeth. This is why a soft-bristled brush is always the smartest choice for protecting your enamel and avoiding what causes tooth sensitivity.
The Hidden Connection Between Your Gums and Sensitivity
While we often blame enamel wear for tooth sensitivity, another major culprit is hiding right where your teeth meet your gums. If you've ever felt that zinging pain concentrated right at the gumline, you're likely dealing with receding gums. This is exactly what it sounds like: your gum tissue has started to pull back, exposing the root of your tooth.
Think of it this way: the top part of your tooth—the crown—is shielded by a tough layer of enamel. The root, however, is covered by a much softer, more porous material called cementum. When your gums recede and expose this layer, it creates a superhighway for hot, cold, or sugary foods to hit the nerve deep inside your tooth.
What Makes Gums Recede?
So, why do gums start to pull away in the first place? It’s not just a random occurrence; there are specific triggers that leave those sensitive roots vulnerable. Getting to know them is the first real step toward protecting your gums and keeping that sharp pain at bay.
Here are some of the most common reasons:
- Gum Disease: This is the big one. Gingivitis and its more serious successor, periodontitis, create inflammation that literally destroys gum tissue and the underlying bone that holds your teeth in place.
- Aggressive Brushing: It might feel like you're getting a better clean, but scrubbing too hard or using a stiff-bristled brush can physically wear down your gums over time.
- Teeth Grinding (Bruxism): The constant pressure from clenching or grinding your teeth doesn't just wear down enamel; it can also stress your gums enough to make them retreat.
- Genetics: Sometimes, it's just in the cards. Some of us are born with thinner gum tissue, which unfortunately makes us more prone to recession.
A major French study revealed that 42.2% of adults struggle with tooth sensitivity. The research pointed directly to risk factors like poor oral hygiene, which is a leading cause of the gum problems that lead to this pain.
Understanding https://serenasandiegodist.com/how-receding-gums-can-affect-your-teeth/ is key because it shows that a healthy mouth is about more than just your teeth. Strong gums are just as important as strong enamel when it comes to preventing sensitivity. If you're spotting the early signs of gum trouble, learning how to treat gingivitis at home can be a powerful way to get back on track and protect your smile.
When Sensitivity Signals a Deeper Dental Issue
While worn enamel and receding gums are the usual suspects, that sudden jolt of pain can sometimes be your mouth’s way of sending up a flare. It’s a warning that your tooth sensitivity might stem from a more serious, underlying problem that needs a professional eye.
Ignoring these signals is a gamble, as it can allow a minor issue to snowball into a major one. The key is learning to tell the difference between everyday sensitivity and a true dental red flag that means it's time to call the dentist.
Red Flags That Need a Dentist's Attention
If your sensitivity feels sudden, severe, or is zeroed in on a single tooth, it could be more than just exposed dentin. These are classic signs of issues that simply won't fix themselves and need proper diagnosis and treatment.
Think of sensitivity as a primary symptom for a few bigger problems:
- Cavities (Tooth Decay): A cavity is basically a hole that punches right through your enamel, creating a superhighway to the sensitive dentin layer. This opening gives heat, cold, and sugar a direct path to your tooth's nerves.
- Cracked or Chipped Teeth: Even a hairline fracture, one you can't even see, can expose the delicate inner pulp of the tooth. Pain from a cracked tooth is often tricky—it might come and go, especially when you bite down in just the right spot.
- Failing Dental Work: Over time, an old filling or crown can wear down, break, or become loose. This creates tiny gaps where bacteria and other irritants can seep in and aggravate the nerve.
A crucial clue is lingering pain. If that zinging feeling from hot or cold sticks around for more than a few seconds after you’ve swallowed your coffee or finished your ice cream, it often means the nerve inside the tooth is inflamed or damaged.
Sensitivity After Dental Procedures
It's also completely normal to experience some temporary sensitivity after getting dental work done, like a new filling, a crown, or a professional whitening treatment. This is usually just the tooth and nerve settling down after the procedure.
This discomfort should fade on its own within a few days or, at most, a couple of weeks. But if the pain hangs on for longer or gets worse, that's a sign to give your dentist a call and let them know.
Finding Real Relief for Sensitive Teeth
Living with that sudden, sharp pain of tooth sensitivity is frustrating, but you don’t have to just put up with it. Real, lasting relief is absolutely within reach. It often starts with simple changes to your daily routine and can be supported by professional treatments that protect your teeth for the long haul.
The key is to first understand what’s causing the discomfort. Once we know the "why," we can find the right "how." By combining smart at-home care with your dentist's guidance, you can finally calm those overactive tooth nerves and get back to enjoying a cold drink or a hot coffee without wincing.
Starting with At-Home Solutions
Your first line of defense is right on your bathroom counter. A few simple swaps in your oral hygiene products can make a world of difference for mild to moderate sensitivity. These changes work in one of two ways: they either block the pain signals from reaching the nerve or help rebuild your tooth’s natural protective layers.
Here are a few strategies that genuinely work:
- Switch to a Desensitizing Toothpaste: Keep an eye out for toothpastes with active ingredients like potassium nitrate or stannous fluoride. Potassium nitrate is the real star here—it works by soothing the nerves inside your teeth, making them far less likely to fire off those pain signals.
- Use a Soft-Bristled Brush: Brushing too hard, especially with stiff bristles, is a major culprit behind enamel wear and gum recession. A soft-bristled brush cleans your teeth just as well without causing any extra damage.
- Add a Fluoride Rinse: Using a fluoride mouthwash every day helps strengthen your enamel, almost like giving it a shield against acid. If you want to dive deeper into this, you can learn more about the effects fluoride treatments can have on your teeth.
Comparing Treatments for Tooth Sensitivity
With so many options out there, it can be tough to know where to start. This table breaks down some of the most common at-home and professional treatments to help you see what might work best for your situation.
| Treatment | How It Provides Relief | Best For |
|---|---|---|
| Desensitizing Toothpaste | Contains compounds (potassium nitrate) that block pain signals from traveling to the tooth's nerve. | Mild to moderate, widespread sensitivity |
| Fluoride Rinse/Varnish | Strengthens and remineralizes tooth enamel, making it more resistant to acid and triggers. | General sensitivity and cavity prevention |
| Dental Bonding | A dentist applies a tooth-colored resin to cover exposed, sensitive root surfaces. | Severe sensitivity in specific areas |
| Gum Graft | Surgically restores gum tissue over receded areas, protecting the exposed tooth root. | Sensitivity caused by significant gum recession |
Ultimately, the right choice depends on the root cause of your sensitivity. While at-home care is a great starting point, a professional diagnosis is the surest way to get effective, targeted relief.
When to Seek Professional Dental Care
If you’ve tried the at-home remedies and still find yourself flinching at every cold breeze or sweet treat, it’s time to call your dentist. The same goes for any sensitivity that feels severe or sharp. Your dentist has the tools and expertise to pinpoint the exact cause and recommend treatments that go far beyond what you can buy at the store.
Pay close attention to persistent or intense sensitivity that's isolated to a single tooth. This can be a red flag for a bigger problem, like a hidden cavity, a cracked tooth, or an infection. Don't wait for the pain to become unbearable.
Professional treatments might involve painting a high-concentration fluoride varnish directly onto the sensitive spots or applying dental bonding material to seal and protect exposed root surfaces. These options create a durable barrier, giving you immediate and long-lasting relief from that painful jolt.
Got Questions About Tooth Sensitivity? We’ve Got Answers.
We’ve dug into the main reasons teeth become sensitive, but you probably still have a few questions rattling around. Let's tackle some of the most common ones we hear from patients every day.
Can Tooth Sensitivity Just Go Away on Its Own?
Sometimes, yes—but usually only if it’s mild and temporary. If you’ve just had a dental cleaning or ate something super acidic, you might feel a little sensitivity that fades in a day or two.
But if the cause is something more permanent, like worn-down enamel or receding gums, the problem won't fix itself. Once that sensitive inner layer of your tooth (the dentin) is exposed, it stays exposed. Without changing your habits or getting some help from your dentist, the sensitivity will likely stick around or even get worse.
Does Teeth Whitening Make Sensitivity Worse?
It definitely can, at least for a little while. The whitening agents in most products are peroxides, which can seep through your enamel and temporarily irritate the nerve inside your tooth.
The good news is that this kind of sensitivity is almost always temporary and stops once you finish the whitening treatment. A great pro tip: try using a desensitizing toothpaste for a week or so before you start whitening and continue using it throughout the process. It can make a world of difference.
Are Some People More Prone to Sensitive Teeth?
Absolutely. It’s not always about what you do; sometimes, it’s just the luck of the draw. Several things can make you more likely to deal with sensitivity:
- Your Genes: Some of us are just born with thinner enamel, which means there's less of a protective barrier over the dentin.
- Your Diet: If you love acidic foods and drinks (think citrus, soda, and wine), your enamel can wear away much faster.
- Other Health Issues: Conditions like acid reflux (GERD) constantly expose your teeth to stomach acid, while grinding your teeth at night (bruxism) can wear them down prematurely.
If you're struggling with this, know that you are far from alone. A major European study revealed that over half of all adults experience dentin hypersensitivity. What’s more, a staggering 98% of them showed signs of dental erosion, which is a key culprit. You can read more about this in the full study on tooth sensitivity prevalence.
When Should I See a Dentist for My Sensitivity?
It's time to make an appointment if your sensitivity is sharp, hangs around for more than a week, or seems to be coming from one specific tooth.
Definitely don't wait if it's paired with other symptoms like pain when you bite down, swollen gums, or if you can see a chip or crack. Those are red flags that could point to a bigger problem that needs a professional eye.
Tired of wincing every time you have a cold drink? If you want to get to the bottom of your tooth sensitivity and find a real solution, the team at Serena San Diego Dentist is here to help. Schedule your appointment today and get back to enjoying your favorite foods without the pain.