When you think about oral cancer, the first signs aren't always dramatic. They're often subtle changes that are easy to dismiss. The most common red flags are things like sores that just won't heal after two weeks, unusual red or white patches inside your mouth, or any strange lumps or thickened spots. These are your body's early warning system, signaling that something is off and needs a professional look.
Why Early Detection Is Your Best Defense
Your mouth is a familiar landscape; you know what feels normal. So, when a small, painless sore sticks around too long or a weirdly colored patch appears out of nowhere, it's a significant sign. The idea isn't to scare you, but to give you the knowledge to act quickly and without hesitation.
Spotting one of these signs is not a diagnosis. Think of it as the starting pistol for getting a professional opinion. Finding potential issues early on drastically improves the chances of successful treatment, which makes your own awareness one of the most powerful health tools you have.
What to Look For During a Self-Exam
A quick self-check once a month is a great habit to build. It helps you get to know your own mouth, making it much easier to catch anything unusual.
- Persistent Sores or Ulcers: Any sore, blister, or ulcer on your lip or inside your mouth that doesn't heal within 14 days is a big one. It needs to be checked out.
- Unusual Color Patches: Be on the lookout for bright red patches (erythroplakia) or white patches (leukoplakia). You might see them on your gums, tongue, tonsils, or the lining of your mouth. Sometimes, these can be precancerous.
- Lumps or Thickening: Gently run your tongue along the inside of your cheeks and the floor of your mouth. Feel for any new lumps, bumps, or areas where the tissue feels thicker or rougher than the surrounding area.
- Pain or Numbness: Unexplained tenderness, pain, or a feeling of numbness anywhere in your mouth or on your lips is another key sign to pay attention to.
To make it even simpler, here's a quick breakdown of what to keep an eye out for.
Quick Guide to Common Oral Cancer Symptoms
This table categorizes the most frequent warning signs by type, helping you quickly identify potential symptoms.
| Symptom Category | Specific Signs to Look For | What It Might Feel or Look Like |
|---|---|---|
| Visual Changes | Red or white patches (leukoplakia/erythroplakia) | A velvety, flat, or slightly raised patch that doesn't scrape off. |
| Tissue Changes | A sore that bleeds easily or doesn't heal in 2 weeks | An ulcer or canker-sore-like spot that just won't go away. |
| Physical Sensations | Lumps, bumps, or thickening of tissue | A hard, painless lump on the side of the tongue or floor of the mouth. |
| Functional Issues | Difficulty chewing, swallowing, or moving the jaw/tongue | A feeling like something is "stuck" in your throat or a sudden change in your bite. |
| Nerve-Related | Numbness, pain, or tenderness in the mouth or lips | An unexplained tingling or loss of feeling, like a dental anesthetic that won't wear off. |
Remember, this guide is for awareness. Only a professional can provide a diagnosis.
The Role of Your Dentist in Screening
While self-exams are a fantastic first step, they can't replace a professional screening. Your dentist is trained to spot subtle signs you would almost certainly miss. During a routine checkup, they're not just looking at your teeth—they're carefully examining all the soft tissues of your mouth, jaw, and neck.
Regular dental visits are your front line of defense. An oral cancer screening is quick, totally painless, and a standard part of any thorough dental exam. It’s the single best opportunity to catch potential problems when they are smallest and most treatable.
This is exactly why knowing how often you should see a dentist is so crucial for a proactive approach to your health. Keeping those appointments ensures a trained pair of eyes is regularly monitoring your oral health, which offers incredible peace of mind. An early warning sign isn't a reason to panic—it's simply a call to action. It’s your cue to schedule an appointment and get the answers you need to stay healthy.
Reading the Signs: Sores, Lumps, and Patches in Your Mouth

When you're checking your mouth for anything unusual, the first things you’ll probably notice are changes you can see or feel. Learning to tell the difference between a minor issue and a potential red flag is the most important first step you can take.
Think about mouth sores. We all get them. You bite your cheek, you scrape your gum on a tortilla chip, or a canker sore pops up out of nowhere. The real difference between a normal sore and a suspicious one comes down to one simple thing: time.
A regular sore should get better and disappear within a week or two. But if you have a sore that sticks around for more than 14 days without healing, that's a signal you shouldn't ignore. It means something is getting in the way of your body's natural healing process.
What Do Different Colors Mean?
Beyond sores, keep an eye out for any patches of color that just don't look right. Think of the inside of your mouth as a familiar landscape—you’d notice if a strange new spot suddenly appeared.
Here are the two main types of patches to be aware of:
- Leukoplakia: These are tough, whitish, or greyish patches that you can't just wipe away. While most are harmless, some can be a sign of precancerous changes.
- Erythroplakia: These show up as bright red, almost velvety patches. They tend to be more delicate and might bleed easily if you touch them. Erythroplakia is less common, but it has a much higher chance of being precancerous.
Occasionally, you might find a patch that's a mix of both red and white, called erythroleukoplakia. These also carry a higher risk and absolutely need to be checked out by a professional.
The tricky thing is that these patches often don't hurt. Because they’re painless, it’s easy to dismiss them. That's why grabbing a mirror and a good light for a quick self-exam every month is one of the best habits you can get into.
If you do spot white patches, it's a good idea to learn more about what they are. Our guide on leukoplakia and its causes in your mouth can give you a better understanding of what to look for.
What to Feel For: Lumps and Thickening
Not all warning signs are visible. Some you can only find by touch, which is why a hands-on check is just as critical as a visual one.
Run a clean finger along the inside of your cheeks, on your lips, and under your tongue. Your tongue is also incredibly sensitive and can often detect a rough or bumpy spot before you can even see it.
Here’s what you should be feeling for:
- New Lumps or Bumps: Feel for any new growths, especially if they feel firm or seem fixed in place.
- Thickened Areas: Take note of any spots where the tissue feels thicker, leathery, or harder than the surrounding areas.
- Rough or Crusted Spots: Be aware of any new textures that feel crusty or rough against your tongue.
These textural changes could point to abnormal cell growth happening below the surface. Oral cancer is a serious health concern, ranking as the 16th most common cancer worldwide. To put that in perspective, in 2022 there were nearly 389,846 new cases globally, resulting in over 188,000 deaths. This is precisely why catching early signs—like a sore that won't heal, strange bleeding, or trouble swallowing—is so crucial for a better outcome.
By learning what to look and feel for, you become an active partner in your own healthcare. The goal isn't to diagnose yourself, but to know your own body well enough to spot when something is off. Finding a persistent sore, an odd-colored patch, or a new lump is your cue to call your dentist and get it professionally checked.
When Your Body Signals a Deeper Problem

The warning signs of oral cancer aren't always something you can see in the mirror. Sometimes, the biggest clues are about function—subtle shifts in how you chew, swallow, or even speak. It’s easy to brush these things off, but when they stick around, it’s a key sign that something more serious could be going on.
Think of it like the "check engine" light in your car. It doesn't tell you the exact problem, but it’s a clear signal to get a professional to look under the hood. When simple, everyday actions suddenly become difficult or painful, your body is sending you the same kind of message.
Difficulty with Swallowing and Chewing
One of the most concerning oral cancer warning signs is finding it suddenly hard to chew or swallow. This condition, known as dysphagia, can make you feel like food is constantly getting stuck in your throat, or turn chewing into a painful chore.
This isn’t like that one time you swallowed a pill the wrong way; it’s a nagging, persistent feeling. It can happen when a tumor grows in a way that blocks your throat or messes with the muscles you need to eat. Any lasting pain or trouble with eating is something you need to get checked out right away.
Changes in Sensation Numbness or Pain
Your mouth, face, and neck are wired with a complex network of nerves. If a growth starts pressing on or invading these nerves, it can trigger some strange sensations that you should never ignore.
Be on the lookout for any of these sensory changes:
- Unexplained Numbness: A lingering numb spot on your tongue, lips, or chin that feels like dental anesthetic that just won’t wear off.
- Tingling or Tenderness: A "pins-and-needles" or burning feeling that shows up for no good reason.
- Persistent Pain: Chronic pain or tenderness in one specific area of your mouth, face, or neck that isn't connected to an obvious problem like a toothache.
Your sense of taste can also be affected by these sensory shifts. While many things can be behind it, you can learn more about the potential reasons for a metallic taste in your mouth to get a better sense of your overall oral health.
A lump or thickening in your cheek or neck is another major red flag. In particular, a painless lump in the neck is one of the most common first signs of throat cancer and demands an immediate medical evaluation.
Voice Changes and Persistent Sore Throat
Has your voice become hoarse or raspy lately? If that change sticks around for more than two weeks and you don't have a cold or allergies, it could signal an issue with your larynx (voice box).
A sore throat that just won't quit is another key indicator. I'm not talking about the kind that comes and goes with a cold, but a constant irritation that lasts for weeks. You might also have that annoying feeling that something is always stuck in your throat.
Learning to recognize these functional and sensory oral cancer warning signs is just as crucial as spotting the visual ones. These symptoms are your body's way of telling you that something is wrong. Listening to these signals and getting a professional opinion is a powerful step you can take for your health. Don't wait—schedule a dental exam to get the answers and peace of mind you deserve.
Checking Your Jaw, Teeth, and Neck for Clues
When we think about oral cancer warning signs, our minds usually jump to sores or patches inside the mouth. But the clues aren't always confined to those soft, pink tissues. Sometimes, the most telling signs are structural—involving your jaw, teeth, and even your neck.
Think of your jawbone as the foundation holding up your smile. If something starts to compromise that foundation, the structures it supports—your teeth—are going to feel the effects. That’s why a sudden, unexplained change in how your teeth feel is a major red flag.
For example, if you notice your teeth have become loose for no clear reason, don't just write it off. The same goes for dentures that suddenly stop fitting correctly. It might not be just a simple dental issue; it could be a signal that something is wrong with the underlying bone.
Listening to Your Jaw
Pain, stiffness, or swelling in your jaw is more than just an annoyance. While a lot of things can cause jaw discomfort, any symptom that sticks around needs a closer look from a professional.
Think about it—you use your jaw constantly. Any new or unexplained trouble chewing, speaking, or simply moving your jaw is a functional warning sign. These problems can suggest that a growth is getting in the way of the complex muscles and joints that make your jaw work. While common issues can cause some of these feelings, it's important to differentiate. For a look at more benign causes, our guide can help explain why your jaw pops when you open your mouth, but persistent, unexplained pain is in a different category.
A change in your bite—how your upper and lower teeth meet—is another subtle but serious sign. If it suddenly feels like your teeth are out of alignment, a dentist needs to figure out why.
The Critical Neck Check
Expanding your self-exam to include your neck is one of the most important things you can do. A lump in the neck that doesn't go away is one of the most common signs that oral cancer may have spread to the lymph nodes. For many people, this is the very first symptom they notice.
What makes these lumps so easy to miss is that they are often completely painless. Because there’s no pain, it’s easy to ignore it, but a firm, fixed lump that doesn’t disappear within a couple of weeks demands an immediate medical evaluation.
Here’s a quick and simple way to check your neck for anything unusual:
- Relax Your Shoulders: Look straight into a mirror while sitting or standing comfortably.
- Use Your Fingertips: With the pads of your fingers, gently press along both sides of your neck. Start right below your ear and work your way down to your collarbone.
- Check Under Your Jaw: Don't forget to feel along the underside of your jawline.
- Notice Asymmetry: You're feeling for any lumps, bumps, or swollen spots. Pay close attention if one side feels different from the other.
Putting All the Clues Together
A good self-check isn't just about one thing; it's about building a complete picture of your oral health. It’s a full-body approach that includes not just what you see inside your mouth but also what you feel in the structures supporting it.
You're looking for changes in:
- Your Teeth: Are they suddenly loose or shifting?
- Your Jaw: Is there nagging pain, stiffness, or trouble moving it?
- Your Neck: Have you found any new, painless lumps that won't go away?
Spotting any of these oral cancer warning signs isn't a reason to panic. It’s simply a signal to take the most responsible step you can: schedule an exam with your dentist. An expert evaluation is the only way to get a real diagnosis and the peace of mind that comes with it.
Understanding Your Risk and How to Reduce It
Knowing what to look for is the first step, but truly understanding why oral cancer develops is what gives you the power to prevent it. It’s about making informed choices that can dramatically lower your chances of ever facing this disease. While you can't change your genetics, many of the biggest risk factors are tied directly to your daily habits.
Think of it like a set of scales. Certain lifestyle choices can tip the scales toward a higher risk, but proactive, healthy habits can bring everything back into balance.
The Major Risk Factors You Can Control
The overwhelming majority of oral cancer cases trace back to a few preventable behaviors. When we look at the data, two factors stand out far above the rest: tobacco and alcohol.
Tobacco Use: This is the big one. Whether you smoke cigarettes, cigars, pipes, or use smokeless products like dip or chew, you are putting yourself at a significantly higher risk. Tobacco is loaded with carcinogens that directly attack and damage the delicate cells in your mouth and throat.
Heavy Alcohol Consumption: Frequent, heavy drinking acts as a powerful irritant to the tissues in your mouth. Over time, this irritation can make your cells more susceptible to the DNA damage that leads to cancer.
But here’s the most critical takeaway: the real danger emerges when tobacco and alcohol are used together. They don't just add to the risk; they multiply it. Think of them as a destructive team, working together to break down your body's defenses far more effectively than either could alone.
This is why quitting tobacco and drinking in moderation are the single most impactful things you can do for your oral health.
The Rise of HPV in Oral Cancer
In recent years, we've seen a major shift in what's causing certain oral cancers, especially those in the back of the throat (the oropharynx). A significant and growing number of these cases are now linked to the Human Papillomavirus (HPV).
This is a really common virus, and it's often found in younger, non-smoking individuals. Most of the time, your immune system clears an HPV infection without any trouble. However, a few high-risk strains can linger and cause cellular changes that, over many years, can develop into cancer. This is a crucial reminder that everyone, regardless of smoking or drinking habits, needs to be vigilant about oral health.
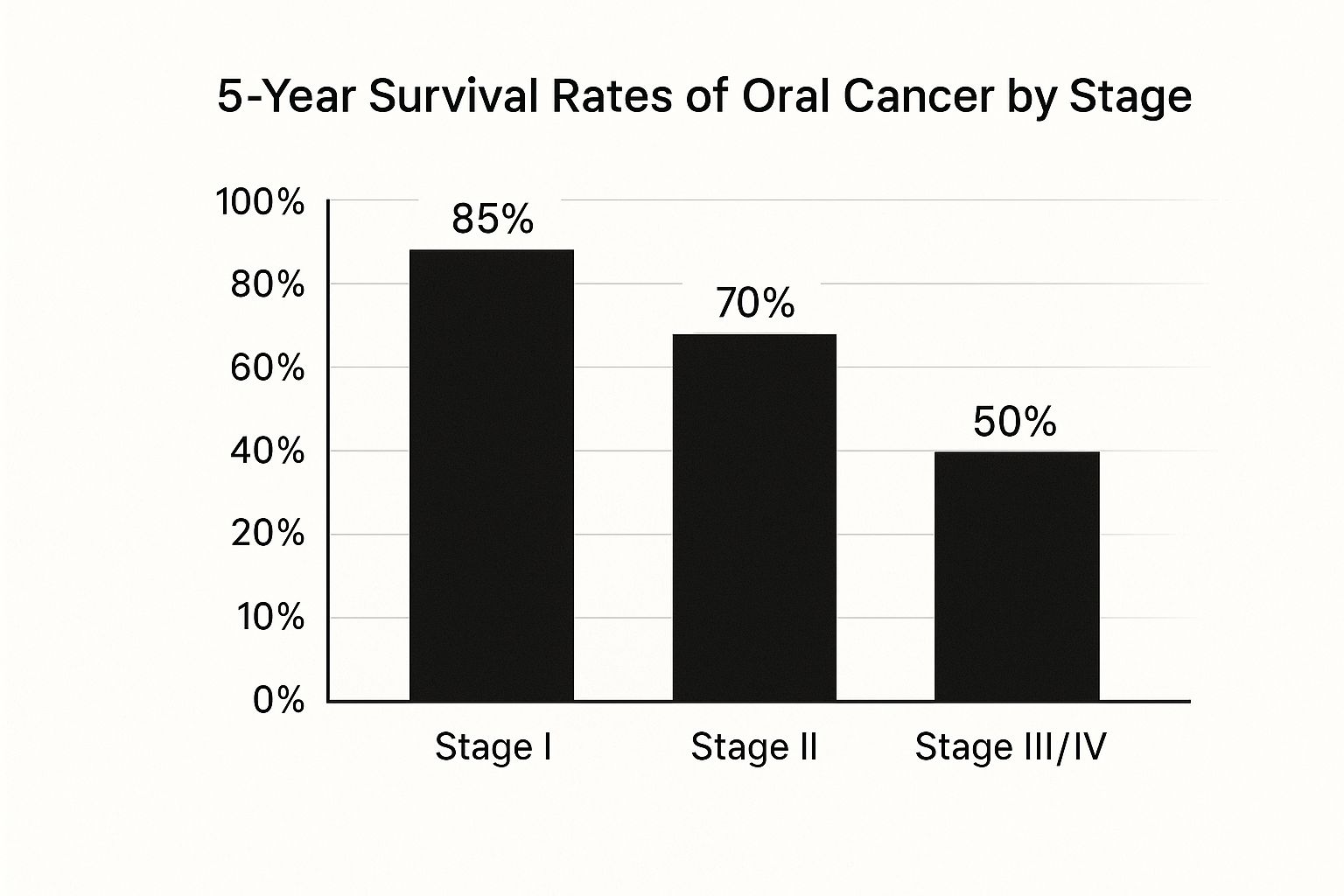
This visual powerfully illustrates why early detection is everything. Spotting cancer at Stage I, when it's localized, results in a much, much higher five-year survival rate compared to when it's discovered at later stages.
Other Contributing Factors
While tobacco, alcohol, and HPV are the primary drivers, several other factors can also tilt the scales. It's important to look at your entire risk profile.
- Sun Exposure: Don't forget your lips! Just like the rest of your skin, your lips are vulnerable to UV radiation, which can lead to lip cancer over time.
- Poor Diet: A diet that’s low in fresh fruits and vegetables can leave your body without the antioxidants and vitamins it needs to fight off cellular damage.
- Family History: If close relatives have had oral cancer, it could signal a genetic predisposition, making regular screenings even more important for you.
- A Weakened Immune System: When your immune system is compromised, it's less effective at fighting off viruses like HPV and can't police the body for abnormal cells as well.
This isn't a rare disease. In the United States alone, an estimated 59,660 new cases of oral and oropharyngeal cancer are expected in 2025. The lifetime risk is roughly 1 in 59 for men and 1 in 139 for women. This gender gap has historically been linked to higher rates of smoking and drinking among men, though these patterns are changing. You can learn more by exploring these oral cancer statistics and their contributing factors.
Oral Cancer Risk Factor Breakdown
To help you connect the dots between risks and actionable prevention, this table summarizes the key factors and what you can do about them. It's designed to give you clear, practical health guidance.
| Risk Factor | How It Increases Risk | Effective Prevention Strategy |
|---|---|---|
| Tobacco Use | Contains dozens of carcinogens that directly damage cellular DNA in the mouth and throat. | Quit completely. Seek support from healthcare providers and use cessation programs. This is the single best step. |
| Heavy Alcohol Use | Irritates oral tissues, making them more vulnerable to carcinogens and DNA damage. | Drink in moderation. Stick to recommended daily guidelines for alcohol consumption. |
| HPV Infection | High-risk strains can cause persistent infections that lead to cancerous cell changes over many years. | Get the HPV vaccine. It's highly effective and recommended for preteens and young adults. |
| Sun Exposure | UV radiation damages the cells of the lips, leading to a specific type of oral cancer. | Protect your lips. Use a lip balm with SPF 30 or higher and wear a wide-brimmed hat. |
| Poor Diet | Lacks the protective antioxidants needed to fight cellular damage and support immune function. | Eat a balanced diet. Load up on a colorful variety of fruits and vegetables. |
Taking these steps isn't just about preventing one disease—it's about investing in your overall, long-term health and well-being.
Your Oral Cancer Questions, Answered
It's completely normal to have questions—and maybe a little anxiety—when you start learning about the warning signs of oral cancer. But getting clear, straightforward answers is the best way to replace that worry with confidence. Let's walk through some of the most common concerns.
Does a Mouth Sore That Won't Heal Automatically Mean I Have Cancer?
No, not at all. While a sore that just won't go away is a major red flag that needs a professional look, the vast majority of mouth sores are harmless. Most are from simple things, like accidentally biting your cheek, a sharp chip, or a common canker sore.
The real key here is time. Your body is an amazing healer, and a typical sore should start feeling better in a few days and be totally gone within two weeks.
Any sore, lump, or strange patch that sticks around longer than that two-week window is your signal to see a dentist. Getting it checked isn't just about catching something serious; it's the fastest way to get peace of mind and confirm everything is okay.
How Often Should I Check My Mouth for Warning Signs?
Getting into the habit of doing a quick self-exam once a month is a fantastic idea. It only takes a minute or two, and doing it regularly helps you get familiar with what’s normal for your mouth. That way, you'll be much more likely to notice if something new pops up.
Think of it as a quick monthly check-in. Here’s a simple way to do it:
- Get a Good View: Stand in front of a well-lit mirror. A small handheld mirror can help you see those hard-to-reach spots.
- Look Around: Carefully inspect the inside of your lips and cheeks, your gums, the roof and floor of your mouth, and all sides of your tongue (top, bottom, and both sides).
- Feel for Changes: With clean fingers, gently feel the tissues inside your mouth. Are there any unusual lumps, bumps, or thick patches that weren't there before?
- Check Your Neck: Gently press along the sides and front of your neck and under your jaw. You're feeling for any new or persistent lumps.
Can My Dentist Screen for Oral Cancer During a Regular Checkup?
Yes, and this is one of the most important parts of your routine visit! An oral cancer screening is a standard, painless part of every comprehensive dental exam. Your dentist has the training to spot subtle changes that are incredibly easy to miss on your own.
During your checkup, your dentist will:
- Carefully examine all the soft tissues of your mouth.
- Gently feel the areas around your jaw, neck, and face for any lumps or firmness.
- Talk with you about any concerns or symptoms you’ve noticed yourself.
This professional screening is one of the best tools we have for catching potential issues early. It’s a huge reason why keeping up with your regular dental visits—at least once a year—is so vital to your overall health.
If I Don't Smoke or Drink, Am I Still at Risk?
It's true that tobacco and heavy alcohol use are the two biggest risk factors, but they aren’t the only ones. Unfortunately, you can still be at risk even if you've never smoked a cigarette or had a drink.
In fact, a growing number of oral cancers, especially those in the back of the throat (oropharyngeal cancers), are now linked to the Human Papillomavirus (HPV).
Other things can also increase your risk, including:
- A diet that's low in fruits and vegetables.
- A weakened immune system.
- A family history of oral or other cancers.
- Frequent, unprotected sun exposure on your lips.
This is exactly why everyone, regardless of lifestyle, should know the warning signs and get screened regularly. Awareness and vigilance are truly your best defense.
Don't let fear or uncertainty keep you from getting the answers you need. The single most important thing you can do is have a professional take a look. At Serena San Diego Dentist, our team is here to give you a thorough, compassionate screening and the peace of mind that comes with it.
Contact us today to schedule your comprehensive dental exam and oral cancer screening. Visit https://serenasandiegodentist.com to book your appointment.



