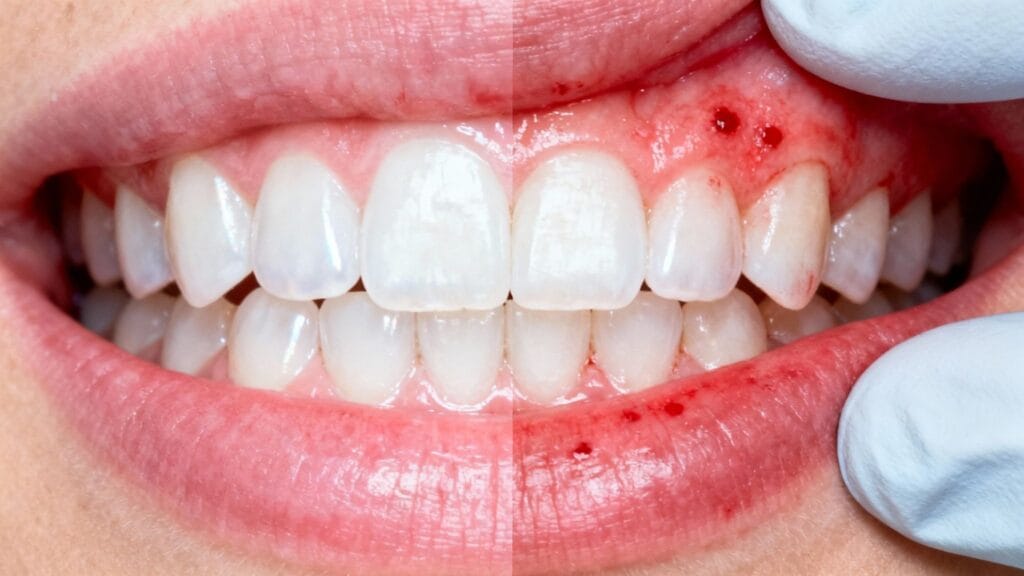
Think of your gums as the foundation for your teeth. When that foundation is compromised, the whole structure is at risk. The earliest warnings of gum disease are often subtle—so subtle, in fact, that most people brush them off as normal.
But a little pink in the sink after you brush? That's not normal. It's one of the first quiet whispers that something is amiss.
Your Guide to Gum Disease Warning Signs
The signs of gum disease are a bit like a fire alarm. At first, you might get a quiet, intermittent beep—a little tenderness or some bleeding when you floss. It's easy to ignore. But if you don't address the source, that quiet beep eventually becomes a full-blown, undeniable siren, signaling a much bigger problem.
Understanding what to look for is the most powerful tool you have. In sunny San Diego, where smiles are always on display, it's easy to overlook small changes in your oral health. But catching these signs early is the key to stopping gum disease in its tracks.
The First Red Flags: Early Warnings
The initial stage of gum disease is called gingivitis. Think of it as a low-level inflammation caused by plaque bacteria camping out along your gumline. The good news? At this point, it's completely reversible with the right care.
Here’s what to keep an eye out for:
- Bleeding Gums: This is the big one. If your gums bleed when you brush or floss, even a tiny bit, they're inflamed. Healthy gums don't bleed.
- Swollen or Puffy Gums: Take a good look in the mirror. Healthy gums are firm, pale pink, and fit snugly around your teeth. If they look reddish, purplish, or puffy, that's a sign of irritation.
- Persistent Bad Breath (Halitosis): We all have "morning breath," but if you find that bad breath lingers all day despite brushing and using mouthwash, it might be from bacteria thriving deep in your gum pockets.
It's crucial to remember that gum disease is often painless in its early stages. You can't rely on discomfort to tell you something is wrong. Those visual cues—the redness, the swelling, the bleeding—are your most reliable early indicators.
Spotting these symptoms isn't a reason to panic. It’s simply a call to action. Stepping up your home care and booking a check-up with your dentist can often turn things around completely, bringing your gums back to perfect health. Letting it slide, however, is what allows the problem to escalate into something far more serious and permanent.
To help you tell the difference, let's compare what you might see in the beginning versus what happens if the disease progresses.
Early vs. Advanced Gum Disease Warning Signs
This table breaks down the initial, often mild signs of gingivitis against the more severe symptoms of periodontitis. It's a quick way to gauge where you might be on the spectrum.
| Symptom | Early Stage (Gingivitis) | Advanced Stage (Periodontitis) |
|---|---|---|
| Gum Appearance | Red, slightly swollen, or puffy. | Bright red, purplish, or very swollen. Gums may pull away from teeth. |
| Bleeding | Bleeds easily during brushing or flossing. | Spontaneous bleeding may occur; significant bleeding with any touch. |
| Teeth | No noticeable changes. | Teeth may look longer (receding gums), shift position, or feel loose. |
| Pain/Sensitivity | Usually painless, maybe mild tenderness. | Gums may be tender or painful; chewing can become uncomfortable. |
| Breath | Persistent bad breath (halitosis) may be present. | Chronic, severe bad breath that doesn't go away. |
| Other Signs | No pus or abscesses. | Pus may be visible between teeth and gums; painful abscesses can form. |
Seeing your symptoms in the "Early Stage" column is a sign to act now and reverse the damage. If you're noticing anything from the "Advanced Stage" column, it's time to see a dentist immediately to prevent further harm.
Understanding the Two Stages of Gum Disease
Gum disease doesn't just show up one day out of the blue. It’s a slow burn, a progressive condition that moves through two main stages, each with its own set of problems and consequences. Here at Serena San Diego Dentist, we often tell our patients to think of it like a small, manageable campfire versus a wildfire that’s raging out of control.
Knowing the difference is everything. If we can catch this thing early, we can often stop it in its tracks and prevent the kind of damage that you can't undo later.
Stage 1: Gingivitis — The Reversible Warning
The first stop on the road is gingivitis. This is your campfire. It all starts with plaque—that sticky, fuzzy film of bacteria that builds up along your gumline. When it sits there, your immune system fires up to fight it off, which causes inflammation.
That inflammation is what you see as the early signs of gum disease. Your gums might look a little red and puffy, and you’ll probably notice some bleeding when you brush or floss. The good news? At this stage, the problem is only in the soft gum tissue. The bone and ligaments holding your teeth in place are still perfectly fine.
The most important thing to know about gingivitis is that it's completely reversible. With some diligent brushing and flossing at home, plus a professional cleaning, we can put out this campfire before it ever has a chance to spread.
This infographic gives you a great visual of how those early, subtle signs can escalate if they aren't addressed.
You can clearly see the difference between the initial warnings and the more serious indicators that tell us something much deeper is going on.
Stage 2: Periodontitis — The Destructive Wildfire
Now, if that gingivitis is ignored, the inflammation doesn’t just go away. This is where the campfire jumps the fire line and becomes a wildfire. The condition has now progressed to periodontitis, and this is a much, much more serious problem.
In this stage, that constant inflammation causes your gums to literally pull away from your teeth, which creates little spaces we call "pockets." These pockets are bad news. They become breeding grounds for bacteria, trapping plaque deep below the gumline where your toothbrush has no hope of reaching.
As your immune system continues its fight, it releases enzymes that, along with the toxins from the bacteria, actually start destroying the bone and tissue that hold your teeth in place. It's a destructive cycle that leads to some serious consequences:
- Deeper Gum Pockets: Those small spaces get bigger and bigger, collecting more bacteria.
- Bone Loss: The actual jawbone that supports your teeth begins to dissolve away.
- Loose Teeth: With their foundation crumbling, teeth start to feel wiggly.
- Tooth Loss: Eventually, if enough bone is lost, teeth can fall out on their own or may need to be removed.
Here's the critical difference: unlike gingivitis, the damage from periodontitis is permanent. While professional treatment can halt the disease and prevent it from getting worse, the bone and tissue that have been lost are gone for good. You can get a deeper look at how this silent but deadly condition affects your teeth in our detailed guide on periodontitis. This is exactly why catching those early warning signs is your absolute best defense.
A Deeper Look at the Top 10 Gum Disease Symptoms
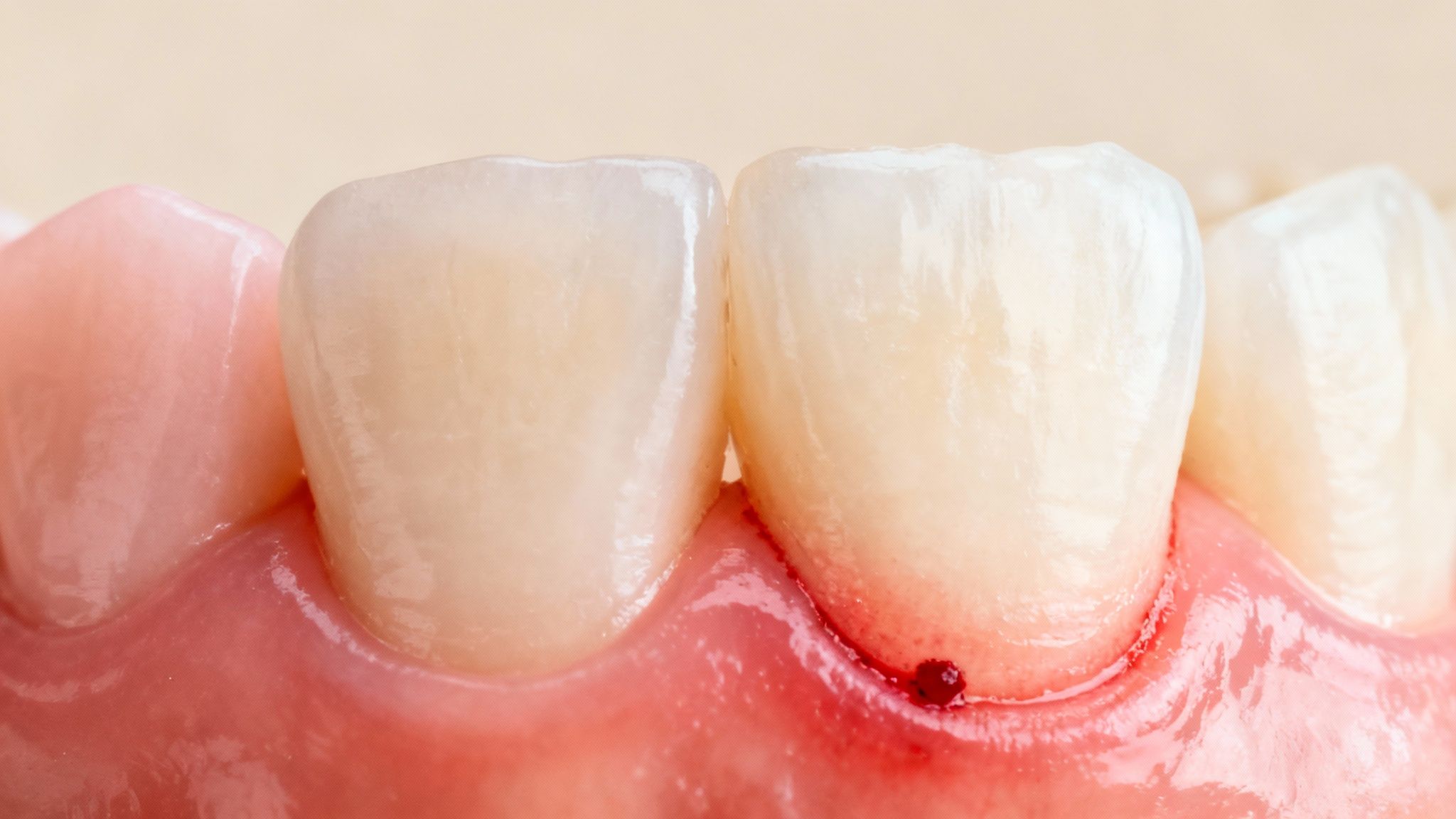
Spotting the early signs of gum disease is your best defense in protecting your smile. But when you understand why these symptoms are happening, you can take action with confidence. Let's walk through the ten most common signs, connecting what you see on the surface to what’s really going on beneath the gumline.
1. Gums That Bleed Easily
This is the classic canary in the coal mine for gum health. Seeing a bit of pink in the sink when you brush or floss isn't normal—it's your body sending out an S.O.S.
The bleeding is a direct result of inflammation. When plaque bacteria build up, your immune system rushes extra blood to your gums to fight off the infection. This makes the tissue swollen and fragile, causing it to bleed with even the slightest touch. If this sounds familiar, you can learn more about how to address bleeding gums in our detailed guide.
2. Red, Swollen, or Tender Gums
Healthy gums are supposed to be firm, pale pink, and fit snugly around your teeth like a turtleneck. If they look red and puffy or feel tender, that’s a clear signal of gingivitis.
This swelling is part of the same inflammatory response. To contain the bacterial assault, the tiny blood vessels in your gums expand and fill with fluid, causing that puffy, irritated appearance.
3. Persistent Bad Breath
I'm not talking about garlic bread or your morning coffee breath. This is the kind of chronic bad breath (halitosis) that lingers long after you've brushed and flossed.
That unpleasant odor is often caused by the waste products from bacteria thriving below the gumline. As they break down food particles, they release smelly sulfur compounds that mouthwash can only mask for a little while.
4. Receding Gums
Ever look in the mirror and think your teeth seem longer than they used to? That's a classic sign of gum recession, a serious red flag that gum disease is progressing.
As the inflammation becomes chronic, the gum tissue literally starts to pull away from the tooth, exposing the root. This is more than just a cosmetic problem; it creates deep pockets where even more bacteria can hide, further damaging the tooth's support system.
The global burden of periodontal diseases is substantial, with 89.6 million new cases recorded annually and over 1 billion people living with the condition in 2021. These statistics highlight how common signs of gum disease—like bleeding during brushing, inflammation, and tooth mobility—are worldwide. You can explore the full findings on the global impact of gum disease.
5. Increased Tooth Sensitivity
If you wince when you sip a cold drink or eat something sweet, it could be your gums talking. As they recede, the sensitive dentin layer of your tooth root gets exposed. This layer is full of tiny nerve endings, making it highly reactive to temperature changes and sugar.
6. Painful Chewing
Feeling discomfort or outright pain when you eat can point to serious issues with the bone and ligaments holding your teeth in place. As periodontitis attacks this foundation, the simple pressure from chewing can become painful.
7. Loose or Shifting Teeth
This is one of the most alarming signs of advanced gum disease. If you can wiggle a tooth with your tongue or notice new gaps opening up between your teeth, it means significant, irreversible bone loss has already occurred. The structures meant to anchor your teeth have been severely compromised.
8. Changes in Your Bite
Does your bite suddenly feel… off? Maybe your top and bottom teeth don't seem to line up the way they used to. As teeth become loose from bone loss, they can drift and shift, completely altering your bite alignment.
9. Changes in the Fit of Partial Dentures
If you wear a partial denture, a sudden change in how it fits is a major clue. As your gums recede and the underlying bone changes shape, your once-snug denture can become loose, wobbly, and uncomfortable.
10. Pus Between Your Teeth and Gums
Seeing a yellowish discharge oozing from your gumline is an undeniable sign of a serious, active infection. This pus is a grim mixture of dead white blood cells, bacteria, and tissue debris—proof that your body is in a full-blown war against periodontitis.
The Causes and Risk Factors Behind Gum Disease

Knowing the warning signs of gum disease is one thing, but understanding what’s really going on behind the scenes is how you build a solid defense. The main villain in this story is bacterial plaque—that invisible, sticky film that’s constantly trying to set up camp on your teeth.
If you don't show that plaque the door every day, it hardens into tartar. Think of tartar as a rough, calcified fortress where even more bacteria can hide out and multiply, kicking off the inflammation that leads to gum disease.
But plaque rarely works alone. A whole host of other factors can make it much easier for gum problems to start and get worse, fast.
Major Risk Factors That Tip the Scales
Your lifestyle, family history, and even your overall health all have a say in how well your gums can defend themselves. Some things just make it harder for your body to fight back, giving bacteria the upper hand.
A few of the biggest risk factors include:
- Poor Oral Hygiene: This one is the most direct cause. If brushing and flossing aren't a consistent part of your daily routine, you’re basically rolling out the welcome mat for plaque.
- Tobacco Use: Whether you smoke or chew, using tobacco is one of the most damaging things you can do to your gums. It weakens your immune system’s defenses and reduces blood flow, making it nearly impossible for your gums to heal properly.
- Genetics: It's an unfortunate truth—some of us are just more likely to develop gum disease because of our genes. If it runs in your family, you have to be extra diligent about your oral health.
- Hormonal Changes: Big hormonal shifts during puberty, pregnancy, or menopause can make your gums extra sensitive and much more vulnerable to the bacteria that cause gingivitis.
- Underlying Health Conditions: Certain illnesses, especially diabetes, can make it much harder for your body to control infections anywhere, including your mouth. There's also a well-established connection between gum disease and conditions like heart disease.
Recognizing these risk factors is key. It helps shift the focus from simply reacting to problems to actively preventing them. This is about building a proactive game plan that’s built around your unique health profile.
Understanding your personal risk factors is the smartest way to avoid more serious problems, like the gum recession that often comes with advanced periodontitis. You can find out more about how receding gums can affect your teeth in our detailed guide on the topic.
To help you get a clearer picture, we've put together a table that breaks down these common risk factors and gives you some practical steps you can take to manage them.
Common Risk Factors for Gum Disease and How to Mitigate Them
| Risk Factor | How It Contributes to Gum Disease | Preventive Action You Can Take |
|---|---|---|
| Poor Oral Hygiene | Allows plaque to accumulate and harden into tartar, irritating the gums and causing inflammation. | Brush twice daily with fluoride toothpaste, floss every day, and see your dentist for regular cleanings. |
| Tobacco Use | Weakens the immune system and reduces blood flow to the gums, impairing their ability to fight infection and heal. | Quit smoking or using tobacco products. Your doctor and dentist can provide resources and support. |
| Genetics | Some individuals have a genetic predisposition that makes them more susceptible to gum infections, regardless of hygiene. | Be extra vigilant with home care and schedule more frequent dental check-ups and cleanings if recommended. |
| Hormonal Changes | Fluctuations (e.g., pregnancy, menopause) can increase gum sensitivity and inflammation in response to plaque. | Maintain excellent oral hygiene and let your dentist know about any hormonal changes or if you are pregnant. |
| Diabetes | Uncontrolled blood sugar levels can compromise the body's ability to fight bacteria, making gum infections more severe. | Work with your doctor to manage your blood sugar. Good glycemic control is crucial for gum health. |
| Stress | Chronic stress can weaken the immune system, making it harder for your body to fight off the bacteria causing gum disease. | Practice stress-reduction techniques like exercise, meditation, or mindfulness to support your overall health. |
Taking a proactive approach by managing these risks gives you the best possible chance of keeping your gums healthy for a lifetime.
How Your Dentist Diagnoses and Treats Gum Disease
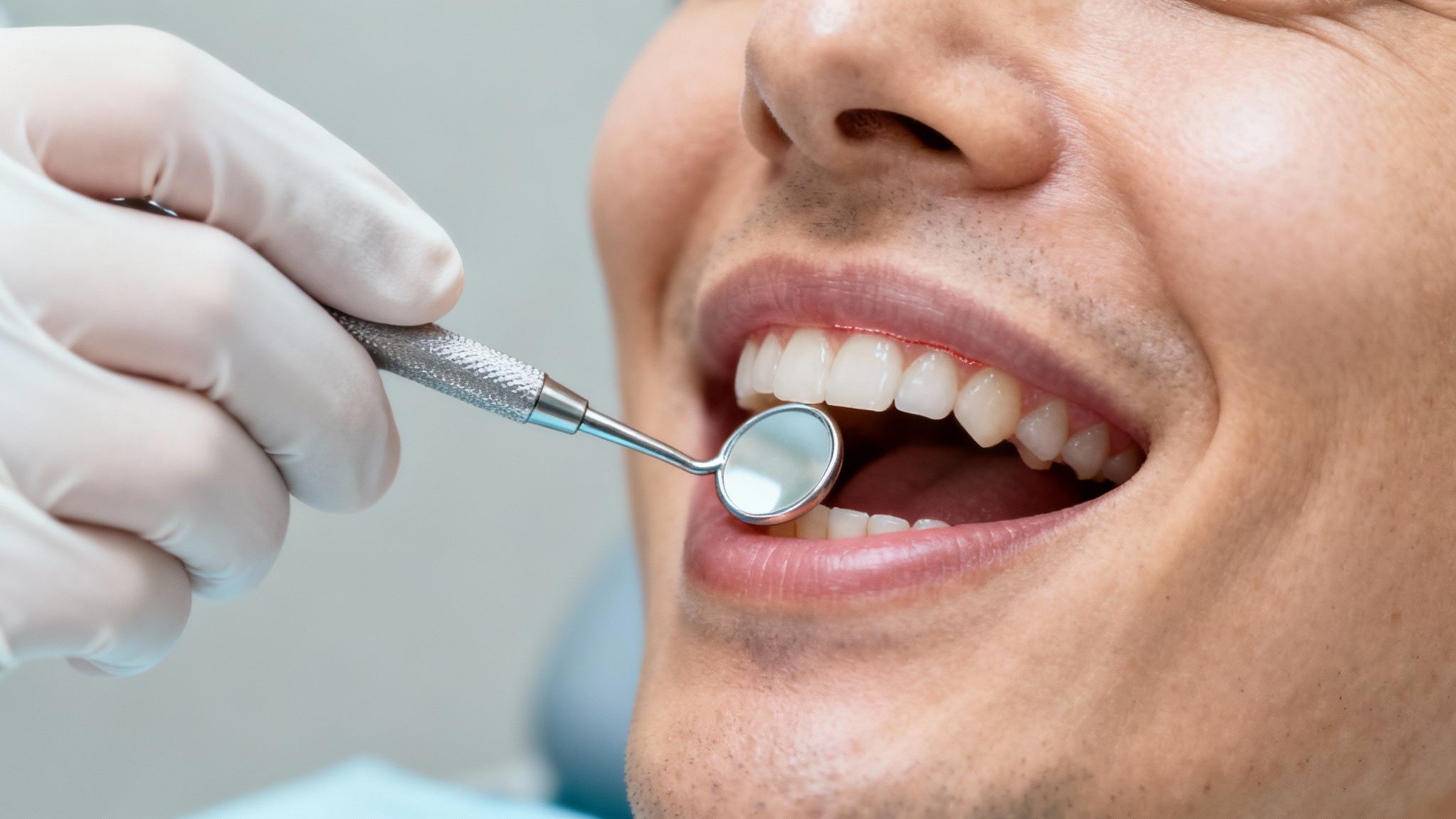
If you've spotted some of the warning signs we've discussed, the next step is to let a professional take a look. We understand a dental visit can feel a little daunting, but knowing what to expect can make all the difference. Let's walk through how we diagnose the issue and show you that effective treatments are available, no matter the stage.
The good news is that the diagnostic process is both straightforward and painless. We'll perform a comprehensive check of your gum health, which involves a few key steps to get a clear picture of any inflammation or damage.
The Diagnostic Process
- Measuring Gum Pockets: We use a tiny, specialized ruler called a periodontal probe to gently measure the small space between your teeth and gums. In a healthy mouth, these "pockets" are typically between 1 and 3 millimeters deep. Pockets that measure deeper than that are often a sign that periodontitis has set in.
- Checking for Bleeding: While we're probing, we'll also keep an eye out for any areas that bleed. Bleeding gums are a classic sign of active inflammation, and it tells us exactly where the trouble spots are.
- Taking Dental X-rays: X-rays are absolutely essential because they show us what's happening beneath the gumline. They give us a clear view of your jawbone’s health and help us spot any bone loss around the teeth—a tell-tale sign of more advanced gum disease.
This isn't just a local issue; it's a global one. As of 2021, over 1 billion individuals worldwide were living with severe periodontitis. This staggering number really underscores why catching it early is so crucial to stopping it from getting worse.
Treatment Options Tailored to You
Once we have a clear diagnosis, we’ll map out a treatment plan that’s tailored specifically to the severity of your gum disease. If we catch it in the early gingivitis stage, a professional cleaning combined with a solid at-home care routine is often all it takes to reverse it completely.
For more advanced cases, the first line of defense is a non-surgical deep cleaning, which you might hear called scaling and root planing. This procedure gets rid of the tough tartar and bacteria that have built up below your gumline. We also smooth out the tooth roots to help your gums heal and reattach properly. You can learn more in our guide on how to know when you need a deep dental cleaning.
In severe cases of periodontitis, surgery might be on the table. Options like flap surgery or bone grafts can help restore tissue that's been lost. While we focus on treating the gum disease itself, it's also wise to be aware of potential complications like a dental abscess, which can happen when oral bacteria issues become severe.
Whatever stage you're at, our primary goal is always the same: to stop the disease in its tracks and save your natural teeth.
Payment and Accessibility at Serena San Diego Dentist
We believe that quality dental care should be accessible. At Serena San Diego Dentist, we accept most major PPO insurance plans for covered services, and our team is happy to help you understand and maximize your benefits. For those who prefer paying out-of-pocket or for treatments not covered by insurance, we offer flexible payment options and financing plans to make your care affordable. Don’t let financial concerns stop you from getting the healthy gums you deserve—contact us to discuss your options.
Your Action Plan for Preventing Gum Disease
Knowing the signs of gum disease is one thing, but actively preventing it is how you truly protect your smile for the long haul. The good news? It's simpler than you might think. Preventing gum disease really boils down to consistent daily habits that stop plaque from ever getting a foothold.
Think of this as your personal game plan—a straightforward way to make your oral health a non-negotiable part of your routine.
Master Your Daily Oral Hygiene
Great gum health starts at home. Your daily routine is, without a doubt, the most powerful weapon you have against the bacteria that cause gum inflammation.
Brush Like You Mean It: You've heard it a million times, but it's true: brush for two full minutes, twice a day. Use a soft-bristled brush and fluoride toothpaste. The key is to angle the brush at a 45-degree angle toward your gumline, using gentle, circular motions to clean where the teeth and gums meet.
Don't Skip the Floss: Flossing is non-negotiable. It’s the only way to clear out the sticky plaque and food debris from between your teeth and just under the gumline—precisely where your toothbrush can't reach. Just once a day makes a huge difference.
Add a Mouthwash Rinse: For an extra layer of defense, consider an ADA-accepted antiseptic mouthwash. It can help kill off bacteria and reduce the plaque that brushing and flossing might have missed.
Lifestyle Choices for Healthy Gums
What you do outside of the bathroom matters just as much. Your everyday choices can either build up your body's defenses against infection or weaken them.
Eating a balanced diet full of vitamins and minerals—especially Vitamin C—gives your gum tissue the nutrients it needs to stay strong and healthy. On the flip side, a diet packed with sugar and starches is like a buffet for plaque-causing bacteria. And it should come as no surprise that using tobacco is one of the single biggest risk factors for gum disease, as it seriously weakens your gums' ability to heal themselves.
Key Takeaway: Your best defense is a one-two punch of meticulous daily cleaning and smart lifestyle choices. Every positive step you take builds a stronger, healthier foundation for your teeth.
Your Top Gum Disease Questions, Answered
We’ve gone through a lot of information, but you probably still have a few questions floating around. That’s completely normal. Here are some of the most common questions we get from patients right here in our San Diego office, along with straight-to-the-point answers from our team.
Can Gum Disease Be Reversed Completely?
Yes, but there’s a catch—it has to be caught early. Gingivitis is completely reversible with consistent, thorough home care and a professional dental cleaning. Think of it as hitting the reset button on your gum health.
Once gingivitis advances into periodontitis, the damage is more serious. The bone and ligaments that hold your teeth in place are permanently damaged. The good news? Professional treatment can stop the disease in its tracks, helping you manage the condition and prevent future tooth loss.
Is It Normal for Gums to Bleed When I Floss?
Absolutely not. Bleeding is never a sign of healthy gums, whether you’re brushing or flossing. In fact, it's one of the earliest and most common warning signs of gum disease.
Think of it as an alarm bell from your body, signaling inflammation caused by plaque buildup. The instinct might be to avoid that sensitive spot, but the right move is to clean it gently and thoroughly, and then book a dental visit.
How Is Gum Disease Linked to Other Health Problems?
The health of your mouth is deeply connected to the health of your entire body—it’s not a separate system. A growing body of research shows a powerful link between advanced gum disease and other serious health conditions.
The bacteria and chronic inflammation from periodontitis can travel through your bloodstream, contributing to major issues like heart disease, stroke, and difficulties managing diabetes. Taking care of your gums isn't just about your smile; it's a critical part of your overall well-being.
If you're noticing any of these signs or just have more questions, please don't wait for things to get worse. The expert team at Serena San Diego Dentist is ready to give you a complete evaluation and a care plan that’s right for you. Schedule your consultation today by calling us or visiting https://serenasandiegodentist.com.