If you're trying to figure out if you need a root canal, the best thing you can do is listen to your body. Specifically, your tooth. Is it a deep, throbbing ache that just won't quit? Or a sharp, shooting pain every time you bite down? These are some of the biggest red flags. Another major sign is when the sensitivity from your morning coffee or a scoop of ice cream sticks around long after you've finished. That's a strong signal that the nerve inside your tooth is in serious trouble, and you shouldn't ignore it.
Decoding the Aches: What Your Tooth Pain Is Saying
That nagging pain in your tooth isn't just an inconvenience; it's a built-in alarm system. But here's the thing: not all tooth pain means the same thing. Learning to recognize the specific type of pain you're feeling is the first step toward figuring out if a root canal might be in your future.
The Difference Between Minor Sensitivity and a Major Concern
Let's be clear, a quick, sharp "zing" from a cold drink every now and then is pretty common and not usually a cause for panic. The kind of pain that points to a root canal is a whole different beast. It's often intense, seems to come out of nowhere, and can completely derail your day.
The real tell-tale sign is persistent tooth pain. We're talking about a sensitivity to hot or cold that doesn't just fade away in a few seconds—it lingers. This often happens when there's a serious infection or inflammation deep inside the tooth's pulp. If you're also dealing with swelling, tenderness when you bite, or a tooth that's incredibly sensitive to touch, those are classic signs that the pulp is either infected or dying. This is when your dentist needs to step in to save the tooth.
This chart can help you figure out what your symptoms might mean.
As you can see, both that lingering ache and sharp, sudden pain are clear signs it's time to call your dentist.
Sometimes it can be tough to distinguish between symptoms. This quick comparison can help you make sense of what you're feeling.
Symptom Severity: Is It a Root Canal or Something Else?
| Symptom | Potential Minor Issue (e.g., Cavity, Gum Sensitivity) | Strong Indicator You May Need a Root Canal |
|---|---|---|
| Pain | Sharp, but goes away quickly. Dull ache that is manageable with over-the-counter pain relief. | Constant, severe, throbbing pain. Pain that wakes you up at night. |
| Sensitivity | Lasts for a few seconds after contact with hot/cold. | Lingering pain that lasts for 30 seconds or more after contact with hot/cold. |
| Gum Issues | Gums are slightly red or bleed when you brush. | A pimple-like bump (abscess) on the gum, swelling of the gums, face, or neck. |
| Biting Pressure | Mild discomfort when chewing certain foods. | Sharp, intense pain when biting down or even touching the tooth. |
| Tooth Color | No change in color. | The tooth starts to look darker or discolored compared to surrounding teeth. |
Remember, this table is just a guide. A professional diagnosis from a dentist is always the best course of action.
Pain When Biting or Applying Pressure
Does a jolt of pain shoot through your tooth when you chew, or even when you just tap on it? This could point to a few different problems, but a nasty infection at the root of the tooth is a very likely culprit. When you bite down, the pressure irritates the already inflamed and infected tissue around the tip of the root, causing that sharp pain.
Of course, sometimes this kind of pain comes from physical damage to the tooth itself. You can find out more about the signs and solutions in our guide on what you need to know about tooth cracks.
Key Takeaway: If a toothache is bad enough to wake you up at night or mess with your daily life, that's not something you should just live with. That level of pain is a clear sign the nerve is in distress and needs professional attention before the problem gets worse.
Visible Clues Your Tooth and Gums Are Sending

While a throbbing toothache is a pretty obvious cry for help, it's not the only signal your body sends when an infection is brewing. Sometimes, the most telling signs are the ones you can see right in the mirror. A quick visual check can give you some serious clues that it's time to call the dentist.
One of the first things to look for is localized swelling and redness around a single tooth. We’re not talking about generally irritated gums from flossing too hard. This is different. You’ll notice the gum tissue around one specific tooth is puffy, inflamed, and a much deeper red than the healthy pink tissue nearby. That’s a classic sign that an infection is festering down at the root.
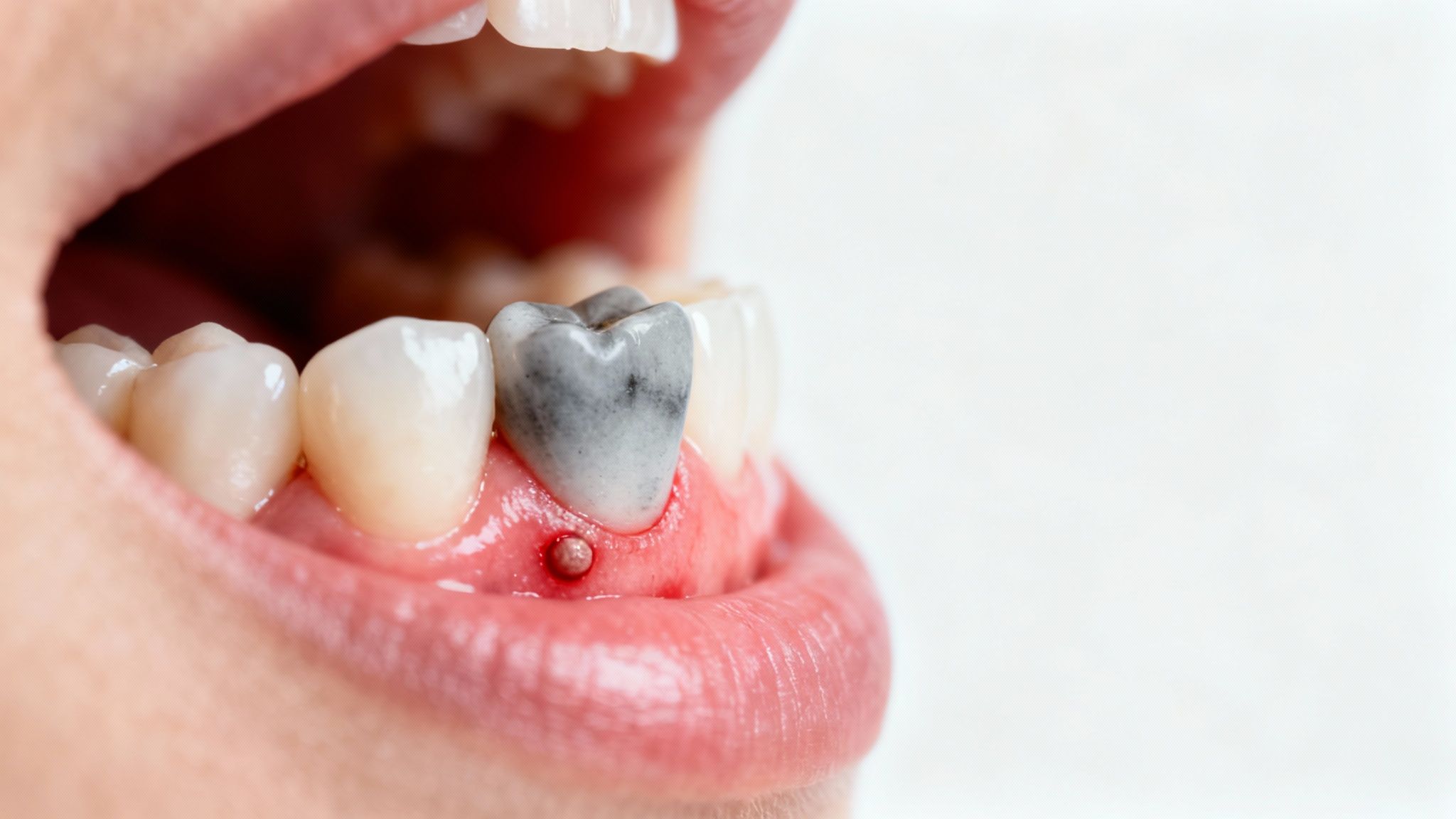
The Pimple on Your Gum
Ever spotted a little bump on your gum that looks like a pimple? That’s no coincidence. This small bump, which dentists call a fistula or gumboil, is a tell-tale sign that your tooth has an abscess and is trying to drain itself.
Think of it as an escape hatch. Your body has created a tiny tunnel to release the pus and pressure building up from the infection at the root. It might even seem to reduce the pain for a little while, but don't be fooled—the infection is still there and actively causing damage. You can learn more about the risks by reading our guide on why a tooth abscess is so dangerous.
An abscessed tooth will not heal on its own. The fistula may come and go, but the source of the infection deep within the tooth must be treated by a dentist to prevent further complications like bone loss or systemic illness.
When a Tooth Changes Color
Another major red flag is when one of your teeth starts to look different from its neighbors. If a tooth begins to turn dark, gray, or even a dingy yellowish-brown, it's often a sign that the nerve inside has died.
When the pulp and blood supply are gone, the internal structure of the tooth starts to break down. Blood pigments leach into the tooth's inner layers, staining it from the inside out. This type of discoloration is a strong indicator of pulp necrosis, a condition that almost always requires a root canal to remove the dead tissue and save the tooth. It’s like an internal bruise, and ignoring it gives the infection a free pass to spread.
When Your Other Senses Signal a Deeper Problem
Have you ever had a persistent bad taste in your mouth that simply won't go away, no matter how much you brush, floss, or swish with mouthwash? It’s a frustrating experience, and it's often more than a minor annoyance. This can actually be one of the less obvious signs that you need a root canal.
While a throbbing toothache and swollen gums are the classic headliners, our other senses—specifically taste and smell—often provide crucial clues about a deep-seated infection. It's easy to dismiss these symptoms as unrelated, but they help paint a much clearer picture of what's really happening below the gumline.
Taste and Smell: The Unmistakable Signs of Infection
When the living tissue, or pulp, inside your tooth gets infected, your immune system rushes white blood cells to the scene to battle the bacteria. This fight creates pus, and if that pus has nowhere to go, it can form a painful pocket called an abscess. Sometimes, this abscess will try to drain itself through a small pimple on your gums or from around the tooth.
That drainage is exactly what causes those unpleasant sensory signals:
- A Persistent Bad Taste: The fluid from the infection often leaves a salty, metallic, or just plain foul taste in your mouth.
- Chronic Bad Breath (Halitosis): The bacteria and decaying tissue produce sulfur compounds, leading to bad breath that oral hygiene can't fix.
If you're noticing either of these, pay attention. It's a strong sign that an active infection is releasing byproducts into your mouth. The problem isn't your brushing habits; it's a symptom of a deeper issue that needs a dentist's expertise.
When you're dealing with a persistent bad taste or breath, it's often your body's way of telling you that an infection is present and needs to be addressed. Ignoring it allows the underlying problem to worsen.
Radiating Aches and Sinus Pressure
Sometimes the trouble isn't just in your mouth. An infection in a top back tooth, for example, can create sensations that seem completely disconnected from your dental health.
Here’s why: the roots of your upper molars sit incredibly close to your maxillary sinuses. When an infection develops at the tip of one of those roots, the inflammation and pressure can push right up into the sinus cavity. This can trigger symptoms that feel just like a sinus infection.
You might experience:
- A dull, constant ache in your cheekbone
- Pressure or tenderness just under your eyes
- A stuffy feeling on only one side of your nose
This connection is often overlooked. We've seen patients who have gone to an ENT specialist for sinus problems, only to find out later that the real culprit was a tooth infection. If you're having sinus-like symptoms alongside any other tooth-related warning signs, it’s a major clue that a root canal might be needed to clear up the infection for good.
The Most Deceptive Sign: No Pain at All
Here's a scenario we've seen play out countless times in our practice: A patient endures a miserable, throbbing toothache for weeks. Then, one morning, they wake up, and like magic, the pain is gone. It's so tempting to think, "Phew, I guess it fixed itself!" and cancel that dental appointment.
But this sudden silence is often the most dangerous red flag.
When that intense pain disappears, it almost never means the infection has healed. It usually means the exact opposite—the infection has gotten so bad that it has killed the nerve inside your tooth. This is a critical point to understand when figuring out if a root canal is in your future.
Why a Pain-Free Tooth Can Be a Major Problem
Think of the nerve, or pulp, as your tooth's built-in alarm system. Its whole job is to scream "Hey, something is wrong in here!" by sending pain signals to your brain.
Once the infection completely overwhelms and destroys that nerve, the alarm gets shut off. You're left with a false sense of security while the bacteria, now completely unchecked, are free to multiply and spread. The party is just getting started for them.
The infection, no longer walled off inside the tooth, can now tunnel its way out the tip of the root and into your jawbone. This is the turning point where a simple tooth problem starts to become a much more serious, body-wide issue.
The absence of pain often signals pulp necrosis, which is the clinical term for the death of the tooth's nerve. While the pain signals are gone, the infection marches on silently, invading the surrounding bone and tissue. This poses a far greater long-term risk to your health.
The Silent Damage Happening Behind the Scenes
Without that nerve sending you frantic distress signals, the infection can cause an incredible amount of damage before you notice anything else is wrong. This quiet invasion can lead to some serious complications that are a lot harder and more expensive to treat than the original toothache ever was.
So, what's really going on?
- Bone Loss: The infection starts dissolving the bone that anchors your tooth, literally eating away at its foundation.
- Abscess Formation: A pocket of pus, called an abscess, can form at the root tip. This is what leads to that classic swollen face, jaw, or neck.
- Systemic Spread: While rare, the bacteria can sometimes get into your bloodstream. This can lead to a life-threatening condition called sepsis.
This is why a tooth that suddenly stops hurting needs to be seen by a professional right away. A dentist can use an X-ray and a few simple tests to confirm if the nerve is dead. Ignoring this deceptive quiet spell is a huge gamble, and you're not just betting on losing your tooth—you're betting against your overall health.
Why You Can't Skip the Dentist's Office
While checking for pain, swelling, and other clues at home gives you a good starting point, it’s not the whole story. Think of it as gathering evidence. You’re building a strong case for why you need an expert opinion, but only a dentist or an endodontist (a root canal specialist) can give you a definitive answer.
We know that the thought of this appointment makes a lot of people nervous. It’s easy to imagine the worst-case scenario. But understanding what actually happens when we diagnose a tooth problem can take a lot of that fear away. A professional evaluation is truly the only reliable path to confirming an infection, figuring out the best treatment, and, most importantly, saving your natural tooth.
What Really Happens During a Diagnostic Exam
When you come into our office with symptoms pointing to a possible root canal, we start a methodical investigation to pinpoint the exact source of your pain. It’s not a scary process; it's just a careful one. In modern dentistry, we use excellent tools like medical documentation software to keep all our findings organized and ensure nothing gets missed.
Here’s a rundown of what we’ll typically do:
- The Tap Test (Percussion): This sounds a lot worse than it is. We simply use a tool to gently tap on a few teeth, including the one giving you trouble. If a specific tooth sends a jolt of sharp pain when tapped, it’s a classic sign of inflammation around the root.
- The Cold Test: We'll touch a small, cold piece of cotton to your tooth for a couple of seconds. A healthy nerve will feel a quick zing that vanishes almost immediately. But if that cold sensation turns into a lingering ache, it tells us the pulp inside is likely inflamed and needs help.
- The X-ray: This is the most crucial piece of the puzzle. A dental X-ray lets us see everything happening beneath the surface, revealing the shape of the root canals and, critically, any signs of infection in the bone. This usually shows up as a small, dark spot right at the tip of the root.
When a Specialist Is the Best Choice
Sometimes, a general dentist will refer you to an endodontist—a dentist who has dedicated their career to saving teeth with procedures like root canals. This is actually becoming more and more common.
According to the American Association of Endodontists, the number of root canals performed by endodontists shot up from 34.6% to 44.4% between 2020 and 2024. That’s a nearly 10% jump in just four years, showing that more people are turning to specialists for their advanced training in handling complex tooth pain.
Expert Insight: Please don't put off a professional evaluation. Getting an accurate diagnosis is the single most important step toward ending your pain and stopping an infection in its tracks. The sooner we identify the problem, the better the odds are of saving your tooth.
Your symptoms are the clues, but a professional diagnosis is what gives you certainty. If any of the signs we’ve discussed sound familiar, it’s time to get a clear answer. If you are looking for expert care in the San Diego area, our team at Serena San Diego Dentist is here to help you get back to feeling like yourself again.
The Real Risks of Ignoring the Warning Signs
It’s tempting to just try and tough it out. We all have busy lives, and the thought of just waiting for the pain to fade is an appealing one. But with a deep tooth infection, that "wait and see" approach is a gamble you don't want to take.
This isn’t about scare tactics. It's about understanding the very real, biological chain of events that kicks off when an infection is left to its own devices. An infected tooth simply cannot heal itself.
Instead, the problem silently gets worse. The infection brewing inside the tooth's pulp almost always leads to a dental abscess—that’s the technical term for the painful, pus-filled pocket that forms at the root tip. This is what's behind that intense, throbbing pain and noticeable facial swelling.
The Progression From Localized to Systemic
Think of an abscess as your body's last-ditch effort to wall off the infection. Unfortunately, it's a losing battle. Eventually, the bacteria start eating away at the surrounding jawbone, a process we call bone loss. This erosion destroys the very foundation holding your tooth, causing it to loosen.
From there, things can get even more serious. The infection isn’t guaranteed to stay put. It can spread to other parts of your head and neck. In rare but life-threatening cases, the bacteria can even enter your bloodstream and trigger sepsis, a body-wide infection.
Key Insight: Ignoring a tooth infection isn't just risking your tooth; it's putting your overall health on the line. This is a serious medical issue that needs a dentist's attention to prevent severe, and sometimes systemic, complications.
The Point of No Return for Your Tooth
Maybe the most common outcome of delaying treatment is simply losing the tooth. A root canal is specifically designed to save a tooth by cleaning out the infection from the inside. But if you wait too long, the infection can cause so much damage to the tooth or the bone supporting it that it’s no longer salvageable.
This forces you into a much more difficult and expensive situation. You might have started with a choice between a root canal vs. an extraction, but waiting often takes that choice away. Learn more about your options for saving your smile in our detailed comparison of root canals versus extractions.
Losing a tooth isn't just about the gap, either. It's about what comes next—a bridge, an implant, or a partial denture. All of these solutions involve far more time, appointments, and expense than simply saving your natural tooth in the first place. When it comes to your teeth, acting sooner is always the better move.
Root Canal FAQs: Your Questions Answered
When you're dealing with tooth pain, a lot of questions can race through your mind. Let's tackle some of the most common ones we hear from our patients in San Diego who are worried they might need a root canal.
Can a Tooth Needing a Root Canal Just Heal Itself?
We wish we could say yes, but unfortunately, that's not how it works. Once the living tissue inside your tooth—the pulp—becomes infected or dies, your body can't clear out the infection on its own.
Without treatment, the problem will only get worse. It can spread and lead to a much more serious and painful dental abscess. A root canal is the only way to get in there, remove the infection, and ultimately save the tooth.
Does Sensitivity to Sugar Automatically Mean I Need a Root Canal?
Not always. More often than not, a sharp, quick pain when you eat something sweet is a classic sign of a simple cavity or even receding gums. It's a definite warning sign to see your dentist.
The key difference is how long the pain lasts. If that sweet sensitivity turns into a lingering, throbbing ache that sticks around long after the cookie is gone, that's a red flag. It could indicate the decay has progressed all the way to the tooth's nerve.
What's the First Thing I Should Do If I'm in Pain?
If you're experiencing severe, throbbing pain or notice any swelling in your face or jaw, that's a dental emergency. You need to call a dentist for an immediate appointment.
In the meantime, you can try to get some temporary relief.
- Gently rinse your mouth with warm salt water.
- Take an over-the-counter pain reliever like ibuprofen or acetaminophen, following the package directions.
- Try your best to avoid chewing on that side of your mouth.
If any of this sounds familiar, please don't put off getting help. Waiting only allows the problem to escalate. At Serena San Diego Dentist, our team is here to give you a clear, honest diagnosis and provide gentle care to get you out of pain and save your natural tooth.
Schedule your consultation with us today and take the first step toward relief.



