You’re back home, the anesthetic is fading, and dinner suddenly feels less simple than it did this morning. You are not just asking what sounds good. You are asking what your healing mouth can handle safely.
That question matters because recovery after dental implant surgery happens in stages. The gum tissue has to settle first. Underneath that, the implant begins the much slower process of bonding with bone, much like a post being set firmly into concrete. That bond does not form overnight. It develops over months, which matches the 3 to 6 month osseointegration timeline detailed earlier in BT Dentist’s implant recovery overview.
So the goal is not only to find “soft foods.” The goal is to match your food choices to what your body is trying to do at each stage of healing. In the first couple of days, food should protect the clot and avoid disturbing the surgical site. In the first week, meals should still be gentle, but they also need to bring in protein, calories, and fluids so your body has the raw materials to repair tissue.
There is another piece patients rarely hear enough about. Pain medicine can slow the bowels and leave you constipated, uncomfortable, and less interested in eating. A smart recovery plan accounts for that too, with enough hydration and the right kinds of easy-to-tolerate foods.
If you keep one idea in mind, let it be this. The best diet after implant surgery is a healing plan, not a menu.
Your First Meal After Dental Implant Surgery
A very common moment happens a few hours after surgery. You get home, sit on the couch, and open the fridge. You may see leftovers, fruit, toast, maybe something crunchy, and suddenly none of it seems safe. That uncertainty is often worse than the soreness.
Your first meal should feel easy, boring, and gentle. That’s a good thing. Right now, your mouth doesn’t need challenge. It needs calm.
Think of the first meal as part of the procedure, not an afterthought. If your implant site is left undisturbed, your body can start the healing work it needs to do. If you chew too soon, sip through a straw, or eat something hot and rough, you can irritate the area when it’s most vulnerable.
Simple rule: if a food needs chewing, crunching, sucking, or careful mouth movement, it’s probably too much for your first meal.
For most patients, the safest first options are things like cool yogurt, a smooth protein shake, applesauce, or a seedless smoothie eaten with a spoon. Temperature matters too. Cool or room temperature foods usually feel better than hot foods right away.
Here’s the mindset I want patients to keep. You are not “being overly careful.” You are actively protecting the work that was just done. If you approach eating that way, choices become easier.
What your body needs right now
Your body is trying to do several things at once:
- Protect the clot so the surgical site stays stable
- Control swelling while the tissue settles
- Start repair with protein, fluids, and rest
- Avoid pressure on the new implant
That’s why this guide follows proper healing phases, not just a random food list.
The First 48 Hours Your Liquid and No-Chew Diet
The first 24 to 48 hours are the most delicate part of recovery. According to Argyle Family Dental’s guidance on soft foods after implant surgery, dental implant surgery success hinges on a phased soft-food diet starting immediately post-procedure, with the first 24-48 hours critical to protect the blood clot. In Phase 1 (hours 1-48), patients must limit intake to cool liquids and no-chew foods like smoothies (seedless fruits only) and yogurt, avoiding straws due to the suction risk that could cause dry socket.
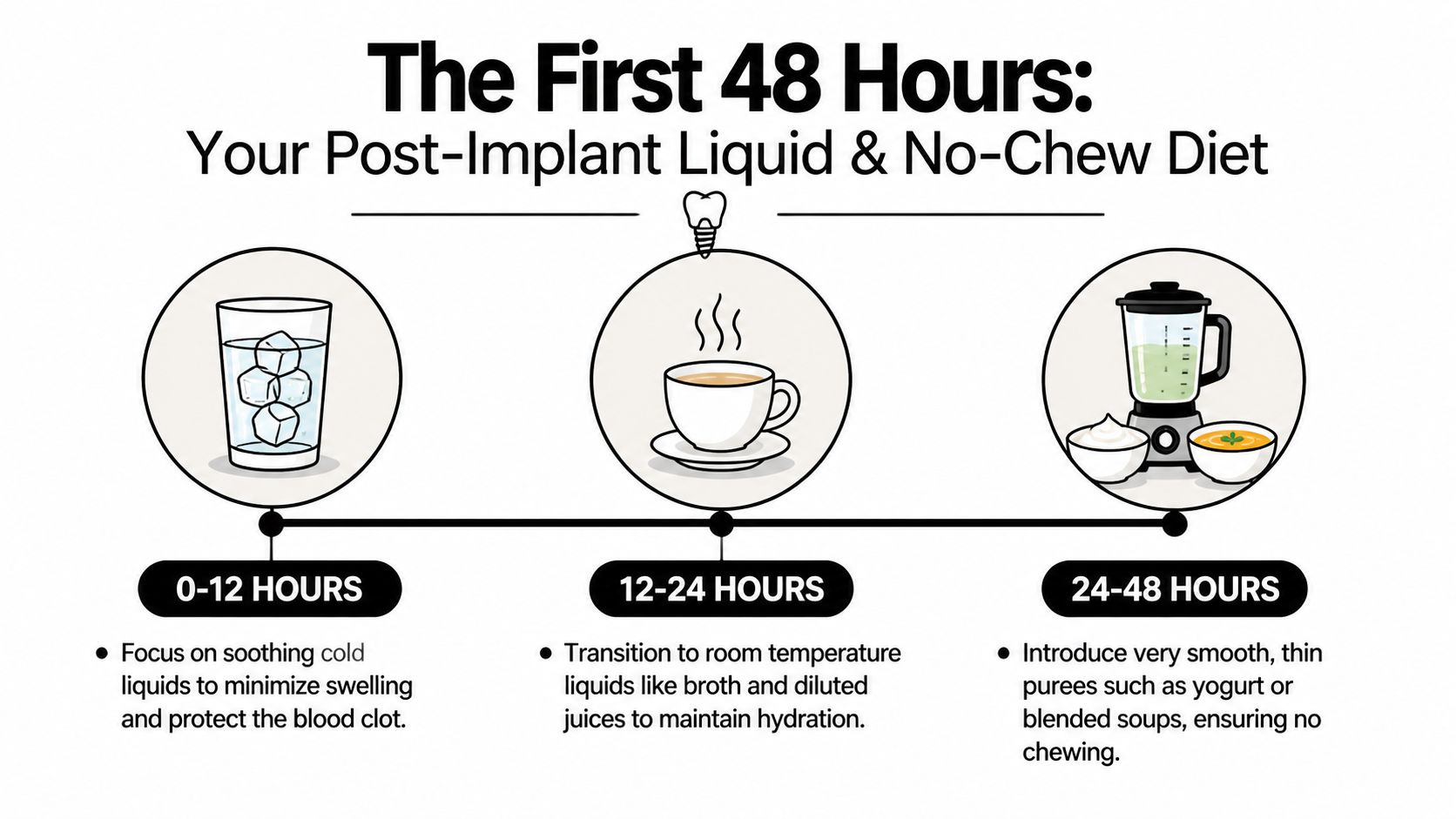
If you remember only one thing from this section, remember this. No straws. The suction can disturb the clot when it needs to stay in place.
What to eat in the first two days
Choose foods that slide down easily and don’t leave bits behind.
- Cool yogurt. Plain or smooth varieties work best.
- Seedless smoothies. Avoid berries with seeds or anything gritty.
- Protein shakes. These can help when you don’t feel like eating.
- Applesauce or pudding. Soft, simple, and easy to tolerate.
- Broth at room temperature or lukewarm. Skip anything steaming hot.
What to avoid right away
Some foods are obvious problems. Others surprise people.
- Straws and suction bottles. These create pressure in the mouth.
- Hot coffee, hot soup, and hot tea. Heat can irritate the area.
- Chunky smoothies with seeds, fruit skins, or ice pieces.
- Anything crunchy like crackers or toast.
- Anything you need to chew, even a little.
Protecting the surgical site is more important than eating a “normal” meal for a day or two.
A practical first-day plan
If you’re hungry but unsure, keep it simple:
- Sip water slowly.
- Have a few spoonfuls of yogurt or applesauce.
- Later, drink a smooth protein shake.
- In the evening, try lukewarm broth.
If your post-op instructions include extra guidance from your surgeon, follow those first. If you also had an extraction or bone work done, your instructions may be even more protective. This tooth removal aftercare page can help you understand the overlap in healing advice.
Navigating Your First Week Introducing Soft Foods
By the third day, many patients feel ready for something more satisfying than liquids. That’s usually the right time to move into soft foods that need very little chewing.

This stage is where nutrition starts doing more visible work. According to Willoughby Dentist Stuart’s guide to soft foods after implant surgery, post-dental implant, a nutrient-focused soft diet combats infection and delayed healing, with protein intake of 1.2-2.0g/kg body weight daily boosting recovery. Key proteins include scrambled eggs, Greek yogurt, and cottage cheese, which are essential as inadequate protein can delay bone integration by 4-6 weeks.
The best soft foods for days 3 through 7
This is the stage where texture matters, but nutrition matters just as much.
- Scrambled eggs for soft, easy protein
- Greek yogurt when you want something cool and filling
- Cottage cheese if you tolerate dairy well
- Mashed potatoes for comfort and easy calories
- Oatmeal once it’s soft and not too hot
- Pureed vegetables such as carrots or squash
- Soft pasta cooked until very tender
Chew on the side opposite the implant if your dentist told you to do so. That one habit can make meals much safer and more comfortable.
Sample meal ideas that work
Patients often know the food list, but they still don’t know how to build a day of eating. Here’s a simple way to approach it:
| Meal | Easy option |
|---|---|
| Breakfast | Scrambled eggs and lukewarm oatmeal |
| Lunch | Pureed vegetable soup and Greek yogurt |
| Snack | Applesauce or cottage cheese |
| Dinner | Mashed potatoes with very soft scrambled egg or soft pasta |
What matters most is consistency. You don’t need creative cooking this week. You need foods that are repeatable and gentle.
Practical meal test: if you can swallow it comfortably without biting down hard, it’s usually in the right category.
A quick visual explanation can also help if you’re someone who learns better by seeing examples:
Where people get confused
The most common mistake in this phase is thinking “soft” means “safe enough.” Some foods are soft but still risky. Bread can gum up and require more chewing than expected. Rice can scatter. Tough pasta can tug at the jaw. Start with the softest version of everything.
Another common mistake is under-eating because chewing feels annoying. That can leave you tired, irritable, and slower to recover. If meals feel like work, lean more on yogurt, eggs, cottage cheese, and smoothies.
Weeks Two and Beyond Reintroducing Texture Safely
You might reach the second week, feel less sore, and assume your mouth is ready for toast, tacos, or a sandwich. That is a common turning point for mistakes. The gums may look calmer on the surface, but the implant is still in the slower stage of healing under the bone.
At this point, your food plan should shift from "what feels soft" to "what supports stable healing." Osseointegration works like setting a post in concrete. The top may seem settled before the base is firm. Your job now is to feed healing tissue well and avoid heavy pressure while that bond strengthens.

Foods that usually fit this stage
You can begin adding more texture, but the food should still break apart easily with a fork or tongue pressure.
- Flaky fish such as soft white fish or salmon
- Moist ground meats that are tender, not browned or chewy
- Soft-cooked pasta with a smooth sauce
- Well-cooked vegetables that mash easily
- Soft grains like oatmeal, quinoa, or rice that has been cooked until tender
- Ripe avocado, banana, or soft tofu for easy calories and gentle texture
A safer way to test new textures
Add one new food at a time.
Chew on the opposite side if your surgeon recommended that. Take small bites. Stop if you notice pressure, clenching, pulling, or the feeling that you need to "test" the implant. That testing habit causes problems because it puts force on an area that is still trying to knit together.
A simple rule helps here. If the food needs a firm first bite, save it for later. If it squishes, flakes, or mashes without much effort, it is usually a better fit for this phase.
Match your meals to the healing work still happening
This stage is less about restriction and more about giving your body the right building materials. Protein helps repair tissue. Calcium and vitamin D support bone turnover. Vitamin C helps with collagen formation in the gums. If meals drift into a pattern of noodles, mashed potatoes, and snack foods, you may feel full but still miss what healing tissue needs.
Pain medicine can create another problem that often gets ignored. Constipation. If that is happening, add soft fiber sources that are still gentle on your mouth, such as oatmeal, blended beans, mashed sweet potato, chia pudding that has softened fully, prunes stewed until soft, or a smoothie with fruit and yogurt. Drink enough water too, because fiber without fluids can make things worse.
Patients who had grafting often need a slower return to texture because there is more healing work happening in the area. If that applies to you, this guide to bone grafting essentials and healing facts explains why extra patience protects the result.
One final tip. Progress should feel boring. Boring is good here. Calm meals, gentle chewing, and steady nutrition usually do more for implant healing than trying to get back to normal too soon.
Foods and Habits to Strictly Avoid for Optimal Healing
Some setbacks happen because a patient eats the wrong thing too soon. Others happen because the food seemed harmless. The problem isn’t always the ingredient itself. It’s the mechanical stress it creates.
According to Dr. Grubb’s explanation of food categories after implant surgery, post-operative guidelines classify foods by mechanical stress. Hard/crunchy foods generate occlusal forces that can cause micro-fractures at the bone-implant interface. Chewy foods create tensile stress, while acidic foods can compromise pH and delay healing. Strict adherence during the initial 10-14 days significantly lowers complication rates.

The no list that matters most
- Hard and crunchy foods like nuts, chips, raw vegetables, crusty bread, and ice
- Sticky foods such as caramel and chewy candy
- Chewy foods like bagels and tough meats
- Acidic foods including citrus and tomatoes if they irritate the area
- Very hot foods and drinks that can aggravate healing tissue
Habits that can also interfere
Food isn’t the only issue. Healing can also be slowed by habits that irritate tissue or work against recovery. Smoking and heavy alcohol use are two big examples your dentist may warn you about after surgery.
If acidic drinks are part of your daily routine, this breakdown of acidic foods and beverages to limit can help you spot common triggers.
A better way to think about restrictions
These limits aren’t punishment. They’re temporary protection for a procedure that’s supposed to last. When patients keep that perspective, it becomes much easier to skip the chips, toast, pizza crust, or steak for a while.
Beyond Food Hydration Supplements and Pain Management
Recovery goes better when you look beyond the plate. Eating the right foods helps, but so do hydration, sensible supplements, and managing medication side effects before they become a problem.
One issue people don’t expect is constipation from pain medication. According to Pinewood Dentistry’s post-implant food guide, a common side effect of post-surgery painkillers is constipation, experienced by up to 45% of dental implant patients. This can be managed with high-fiber soft foods like blended prunes (7g fiber/serving) or mashed avocados (6.7g fiber/fruit), which support gut motility without requiring chewing and can reduce recovery complications.
Hydration that actually helps
Plain water is the foundation. Sip regularly throughout the day rather than trying to catch up all at once. If you want more variety, choose gentle drinks that aren’t overly hot or irritating.
Some patients also like electrolyte support when eating is limited. If you’re comparing options, this resource to compare electrolyte hydration mixes can help you think through ingredients and use cases in a practical way.
Soft-food ways to stay regular
Constipation can make you feel worse even when the implant itself is doing fine. A few food choices can help:
- Blended prunes mixed into a smoothie
- Mashed avocado eaten plain or stirred into soft foods
- Oatmeal if you’re already tolerating it well
- Extra fluids through the day, not just with meals
Recovery is smoother when your meals support both healing in the mouth and comfort in the rest of your body.
What about supplements
If your dentist or physician has recommended supplements, keep them simple and consistent. Vitamin C, calcium, and protein support are often discussed in implant recovery because they align with tissue repair and bone healing. Always use your own care team’s guidance if you take other medications or have medical conditions.
For longer-term care after healing, this page on looking after dental implants and oral health gives a useful overview of maintenance habits.
Your Recovery Checklist and When to Call Your San Diego Dentist
When patients know what’s normal, they feel less anxious. When they know what isn’t normal, they call sooner, which is usually the right move.
A simple recovery checklist
- First 48 hours. Stick with cool liquids and no-chew foods.
- Days 3 through 7. Add soft foods with protein and chew away from the implant if instructed.
- Weeks 2 and beyond. Bring back texture gradually, but stay cautious with pressure.
- Throughout recovery. Keep meals gentle, stay hydrated, and avoid foods that are hard, sticky, chewy, acidic, or very hot.
Call your dentist if something feels off
Reach out if you notice:
- bleeding that doesn’t seem to settle
- pain that gets worse instead of better
- swelling that feels like it’s increasing rather than calming down
- a bad taste, unusual drainage, or other signs that concern you
- trouble eating or drinking because the area feels increasingly irritated
If you’re exploring supportive wellness strategies during healing, a general guide to anti-inflammatory supplements may be a helpful starting point for questions to bring to your healthcare team.
If you need personalized implant care, post-op guidance, or treatment planning, learn more about dental implants in San Diego. Clear instructions and timely follow-up can make recovery feel much more manageable.
If you have questions about what to eat after dental implant surgery, want a second opinion, or need expert implant care in San Diego, Clairemont Mesa, or La Jolla, schedule a consultation with Serena San Diego Dentist. Our team can give you personalized aftercare guidance so you can heal comfortably and protect your new smile.



